Hernia
A hernia is the abnormal exit of tissue or an organ, such as the bowel, through the wall of the cavity in which it normally resides.[1] Hernias come in a number of types.[6] Most commonly they involve the abdomen, specifically the groin.[6] Groin hernias are most common of the inguinal type but may also be femoral.[1] Other hernias include hiatus, incisional, and umbilical hernias.[6] Symptoms are present in about 66% of people with groin hernias.[1] This may include pain or discomfort especially with coughing, exercise, or going to the bathroom.[1] Often it gets worse throughout the day and improves when lying down.[1] A bulging area may occur that becomes larger when bearing down.[1] Groin hernias occur more often on the right than left side.[1] The main concern is strangulation, where the blood supply to part of the bowel is blocked.[1] This usually produces severe pain and tenderness of the area.[1] Hiatus or hiatal hernias often result in heartburn but may also cause chest pain or pain with eating.[3]
| Hernia | |
|---|---|
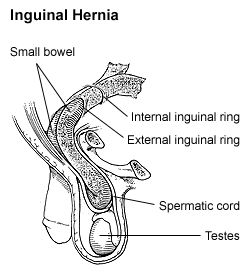 | |
| Diagram of an indirect inguinal hernia (view from the side). | |
| Specialty | General surgery |
| Symptoms | Pain especially with coughing, bulging area[1] |
| Complications | Bowel strangulation[1] |
| Usual onset | < 1 year and > 50 years old (groin hernias)[2] |
| Risk factors | Smoking, chronic obstructive pulmonary disease, obesity, pregnancy, peritoneal dialysis, collagen vascular disease[1][2][3] |
| Diagnostic method | Based on symptoms, medical imaging[1] |
| Treatment | Observation, surgery[1] |
| Frequency | 18.5 million (2015)[4] |
| Deaths | 59,800 (2015)[5] |
Risk factors for the development of a hernia include: smoking, chronic obstructive pulmonary disease, obesity, pregnancy, peritoneal dialysis, collagen vascular disease, and previous open appendectomy, among others.[1][2][3] Hernias are partly genetic and occur more often in certain families.[1] It is unclear if groin hernias are associated with heavy lifting.[1] Hernias can often be diagnosed based on signs and symptoms.[1] Occasionally medical imaging is used to confirm the diagnosis or rule out other possible causes.[1] The diagnosis of hiatus hernias is often by endoscopy.[3]
Groin hernias that do not cause symptoms in males do not need to be repaired.[1] Repair, however, is generally recommended in women due to the higher rate of femoral hernias which have more complications.[1] If strangulation occurs immediate surgery is required.[1] Repair may be done by open surgery or by laparoscopic surgery.[1] Open surgery has the benefit of possibly being done under local anesthesia rather than general anesthesia.[1] Laparoscopic surgery generally has less pain following the procedure.[1] A hiatus hernia may be treated with lifestyle changes such as raising the head of the bed, weight loss, and adjusting eating habits.[3] The medications, H2 blockers or proton pump inhibitors may help.[3] If the symptoms do not improve with medications the surgery known as laparoscopic fundoplication may be an option.[3]
About 27% of males and 3% of females develop a groin hernia at some time in their life.[1] Inguinal, femoral and abdominal hernias were present in 18.5 million people and resulted in 59,800 deaths in 2015.[4][5] Groin hernias occur most often before the age of one and after the age of fifty.[2] It is not known how commonly hiatus hernias occur with estimates in North America varying from 10 to 80%.[3] The first known description of a hernia dates back to at least 1550 BC in the Ebers Papyrus from Egypt.[7]
Signs and symptoms
By far the most common hernias develop in the abdomen, when a weakness in the abdominal wall evolves into a localized hole, or "defect", through which adipose tissue, or abdominal organs covered with peritoneum, may protrude. Another common hernia involves the spinal discs and causes sciatica. A hiatus hernia occurs when the stomach protrudes into the mediastinum through the esophageal opening in the diaphragm.
Hernias may or may not present with either pain at the site, a visible or palpable lump, or in some cases more vague symptoms resulting from pressure on an organ which has become "stuck" in the hernia, sometimes leading to organ dysfunction. Fatty tissue usually enters a hernia first, but it may be followed or accompanied by an organ.
Hernias are caused by a disruption or opening in the fascia, or fibrous tissue, which forms the abdominal wall. It is possible for the bulge associated with a hernia to come and go, but the defect in the tissue will persist.
Symptoms and signs vary depending on the type of hernia. Symptoms may or may not be present in some inguinal hernias. In the case of reducible hernias, a bulge in the groin or in another abdominal area can often be seen and felt. When standing, such a bulge becomes more obvious. Besides the bulge, other symptoms include pain in the groin that may also include a heavy or dragging sensation, and in men, there is sometimes pain and swelling in the scrotum around the testicular area.[8]
Irreducible abdominal hernias or incarcerated hernias may be painful, but their most relevant symptom is that they cannot return to the abdominal cavity when pushed in. They may be chronic, although painless, and can lead to strangulation (loss of blood supply), obstruction (kinking of intestine), or both. Strangulated hernias are always painful and pain is followed by tenderness. Nausea, vomiting, or fever may occur in these cases due to bowel obstruction. Also, the hernia bulge in this case may turn red, purple or dark and pink.
In the diagnosis of abdominal hernias, imaging is the principal means of detecting internal diaphragmatic and other nonpalpable or unsuspected hernias. Multidetector CT (MDCT) can show with precision the anatomic site of the hernia sac, the contents of the sac, and any complications. MDCT also offers clear detail of the abdominal wall allowing wall hernias to be identified accurately.[9]
Complications
Complications may arise post-operation, including rejection of the mesh that is used to repair the hernia. In the event of a mesh rejection, the mesh will very likely need to be removed. Mesh rejection can be detected by obvious, sometimes localized swelling and pain around the mesh area. Continuous discharge from the scar is likely for a while after the mesh has been removed.
A surgically treated hernia can lead to complications such as inguinodynia, while an untreated hernia may be complicated by:
- Inflammation
- Obstruction of any lumen, such as bowel obstruction in intestinal hernias
- Strangulation
- Hydrocele of the hernial sac
- Hemorrhage
- Autoimmune problems
- Irreducibility or Incarceration, in which it cannot be reduced, or pushed back into place,[10] at least not without very much external effort.[11] In intestinal hernias, this also substantially increases the risk of bowel obstruction and strangulation.
Causes
Causes of hiatus hernia vary depending on each individual. Among the multiple causes, however, are the mechanical causes which include: improper heavy weight lifting, hard coughing bouts, sharp blows to the abdomen, and incorrect posture.[12]
Furthermore, conditions that increase the pressure of the abdominal cavity may also cause hernias or worsen the existing ones. Some examples would be: obesity, straining during a bowel movement or urination (constipation, enlarged prostate), chronic lung disease, and also, fluid in the abdominal cavity (ascites).[13]
Also, if muscles are weakened due to poor nutrition, smoking, and overexertion, hernias are more likely to occur.
The physiological school of thought contends that in the case of inguinal hernia, the above-mentioned are only an anatomical symptom of the underlying physiological cause. They contend that the risk of hernia is due to a physiological difference between patients who suffer hernia and those who do not, namely the presence of aponeurotic extensions from the transversus abdominis aponeurotic arch.[14]
Abdominal wall hernia may occur due to trauma. If this type of hernia is due to blunt trauma it is an emergency condition and could be associated with various solid organs and hollow viscus injuries.
Diagnosis
Inguinal
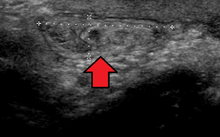
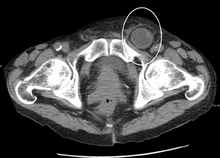
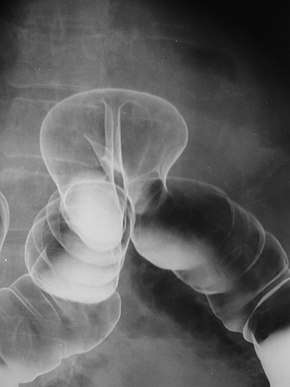
By far the most common hernias (up to 75% of all abdominal hernias) are the so-called inguinal hernias. Inguinal hernias are further divided into the more common indirect inguinal hernia (2/3, depicted here), in which the inguinal canal is entered via a congenital weakness at its entrance (the internal inguinal ring), and the direct inguinal hernia type (1/3), where the hernia contents push through a weak spot in the back wall of the inguinal canal. Inguinal hernias are the most common type of hernia in both men and women. In some selected cases, they may require surgery. There are special cases in which the hernia may contain both direct and indirect hernia simultaneously pantaloon hernia, or, though very rare, may contain simultaneous indirect hernias.[15]
Pantaloon hernia (Saddle Bag hernia) is a combined direct and indirect hernia, when the hernial sac protrudes on either side of the inferior epigastric vessels.
Femoral
Femoral hernias occur just below the inguinal ligament, when abdominal contents pass into the weak area at the posterior wall of the femoral canal. They can be hard to distinguish from the inguinal type (especially when ascending cephalad): however, they generally appear more rounded, and, in contrast to inguinal hernias, there is a strong female preponderance in femoral hernias. The incidence of strangulation in femoral hernias is high. Repair techniques are similar for femoral and inguinal hernia.
A Cooper's hernia is a femoral hernia with two sacs, the first being in the femoral canal, and the second passing through a defect in the superficial fascia and appearing almost immediately beneath the skin.
Umbilical
They involve protrusion of intra-abdominal contents through a weakness at the site of passage of the umbilical cord through the abdominal wall. Umbilical hernias in adults are largely acquired, and are more frequent in obese or pregnant women. Abnormal decussation of fibers at the linea alba may contribute.
Incisional
An incisional hernia occurs when the defect is the result of an incompletely healed surgical wound. When these occur in median laparotomy incisions in the linea alba, they are termed ventral hernias. These can be the most frustrating and difficult to treat, as the repair utilizes already attenuated tissue. These occur in about 13% of people at 2 years following surgery.[16]
Diaphragmatic
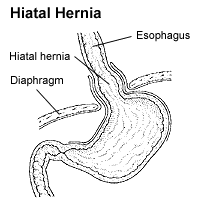
Higher in the abdomen, an (internal) "diaphragmatic hernia" results when part of the stomach or intestine protrudes into the chest cavity through a defect in the diaphragm.
A hiatus hernia is a particular variant of this type, in which the normal passageway through which the esophagus meets the stomach (esophageal hiatus) serves as a functional "defect", allowing part of the stomach to (periodically) "herniate" into the chest. Hiatus hernias may be either "sliding", in which the gastroesophageal junction itself slides through the defect into the chest, or non-sliding (also known as para-esophageal), in which case the junction remains fixed while another portion of the stomach moves up through the defect. Non-sliding or para-esophageal hernias can be dangerous as they may allow the stomach to rotate and obstruct. Repair is usually advised.
A congenital diaphragmatic hernia is a distinct problem, occurring in up to 1 in 2000 births, and requiring pediatric surgery. Intestinal organs may herniate through several parts of the diaphragm, posterolateral (in Bochdalek's triangle, resulting in Bochdalek's hernia), or anteromedial-retrosternal (in the cleft of Larrey/Morgagni's foramen, resulting in Morgagni-Larrey hernia, or Morgagni's hernia).[17]
Other hernias
Since many organs or parts of organs can herniate through many orifices, it is very difficult to give an exhaustive list of hernias, with all synonyms and eponyms. The above article deals mostly with "visceral hernias", where the herniating tissue arises within the abdominal cavity. Other hernia types and unusual types of visceral hernias are listed below, in alphabetical order:
- Abdominal wall hernias:
- Umbilical hernia
- Epigastric hernia: a hernia through the linea alba above the umbilicus.
- Spigelian hernia, also known as spontaneous lateral ventral hernia
- Amyand's hernia: containing the appendix vermiformis within the hernia sac
- Brain herniation, sometimes referred to as brain hernia, is a potentially deadly side effect of very high intracranial pressure that occurs when a part of the brain is squeezed across structures within the skull.
- Double indirect hernia: an indirect inguinal hernia with two hernia sacs, without a concomitant direct hernia component (as seen in a pantaloon hernia).[15]
- Hiatus hernia: a hernia due to "short oesophagus" — insufficient elongation — stomach is displaced into the thorax
- Littre's hernia: a hernia involving a Meckel's diverticulum. It is named after the French anatomist Alexis Littré (1658–1726).
- Lumbar hernia: a hernia in the lumbar region (not to be confused with a lumbar disc hernia), contains the following entities:
- Petit's hernia: a hernia through Petit's triangle (inferior lumbar triangle). It is named after French surgeon Jean Louis Petit (1674–1750).
- Grynfeltt's hernia: a hernia through Grynfeltt-Lesshaft triangle (superior lumbar triangle). It is named after physician Joseph Grynfeltt (1840–1913).
- Maydl's hernia: two adjacent loops of small intestine are within a hernial sac with a tight neck. The intervening portion of bowel within the abdomen is deprived of its blood supply and eventually becomes necrotic.
- Obturator hernia: hernia through obturator canal
- Parastomal hernias, which is when tissue protrudes adjacent to a stoma tract.
- Paraumbilical hernia: a type of umbilical hernia occurring in adults
- Perineal hernia: a perineal hernia protrudes through the muscles and fascia of the perineal floor. It may be primary but usually is acquired following perineal prostatectomy, abdominoperineal resection of the rectum, or pelvic exenteration.
- Properitoneal hernia: rare hernia located directly above the peritoneum, for example, when part of an inguinal hernia projects from the deep inguinal ring to the preperitoneal space.
- Richter's hernia: a hernia involving only one sidewall of the bowel, which can result in bowel strangulation leading to perforation through ischaemia without causing bowel obstruction or any of its warning signs. It is named after German surgeon August Gottlieb Richter (1742–1812).
- Sliding hernia: occurs when an organ drags along part of the peritoneum, or, in other words, the organ is part of the hernia sac. The colon and the urinary bladder are often involved. The term also frequently refers to sliding hernias of the stomach.
- Sciatic hernia: this hernia in the greater sciatic foramen most commonly presents as an uncomfortable mass in the gluteal area. Bowel obstruction may also occur. This type of hernia is only a rare cause of sciatic neuralgia.
- Sports hernia: a hernia characterized by chronic groin pain in athletes and a dilated superficial inguinal ring.
- Velpeau hernia: a hernia in the groin in front of the femoral blood vessels
Treatment
Truss
The benefits of the use of an external device to maintain reduction of the hernia without repairing the underlying defect (such as hernia trusses, trunks, belts, etc.) are unclear.[1]
Surgery
Surgery is recommended for some types of hernias to prevent complications like obstruction of the bowel or strangulation of the tissue, although umbilical hernias and hiatus hernias may be watched, or are treated with medication.[18] Most abdominal hernias can be surgically repaired, but surgery has complications. Time needed for recovery after treatment is reduced if hernias are operated on laparoscopically. However, open surgery can be done sometimes without general anesthesia.
Uncomplicated hernias are principally repaired by pushing back, or "reducing", the herniated tissue, and then mending the weakness in muscle tissue (an operation called herniorrhaphy). If complications have occurred, the surgeon will check the viability of the herniated organ and remove part of it if necessary.
Muscle reinforcement techniques often involve synthetic materials (a mesh prosthesis).[19] The mesh is placed either over the defect (anterior repair) or under the defect (posterior repair). At times staples are used to keep the mesh in place. These mesh repair methods are often called "tension free" repairs because, unlike some suture methods (e.g., Shouldice), muscle is not pulled together under tension. However, this widely used terminology is misleading, as there are many tension-free suture methods that do not use mesh (e.g., Desarda, Guarnieri, Lipton-Estrin, etc.).
Evidence suggests that tension-free methods (with or without mesh) often have lower percentage of recurrences and the fastest recovery period compared to tension suture methods. However, among other possible complications, prosthetic mesh usage seems to have a higher incidence of chronic pain and, sometimes, infection.[20]
The frequency of surgical correction ranges from 10 per 100,000 (U.K.) to 28 per 100,000 (U.S.).[1]
Recovery
Many people are managed through day surgery centers, and are able to return to work within a week or two, while intense activities are prohibited for a longer period. People who have their hernias repaired with mesh often recover within a month, though pain can last longer. Surgical complications include pain that lasts more than three months, surgical site infections, nerve and blood vessel injuries, injury to nearby organs, and hernia recurrence. Pain that lasts more than three months occurs in about 10% of people following hernia repair.[1]
Epidemiology
About 27% of males and 3% of females develop a groin hernia at some time in their lives.[1] In 2013 about 25 million people had a hernia.[21] Inguinal, femoral and abdominal hernias resulted in 32,500 deaths globally in 2013 and 50,500 in 1990.[22]
References
- Fitzgibbons RJ, Jr; Forse, RA (19 February 2015). "Clinical practice. Groin hernias in adults". The New England Journal of Medicine. 372 (8): 756–63. doi:10.1056/NEJMcp1404068. PMID 25693015.
- Domino, Frank J. (2014). The 5-minute clinical consult 2014 (22nd ed.). Philadelphia, Pa.: Wolters Kluwer Health/Lippincott Williams & Wilkins. p. 562. ISBN 9781451188509. Archived from the original on 2017-08-22.
- Roman, S; Kahrilas, PJ (23 October 2014). "The diagnosis and management of hiatus hernia". BMJ (Clinical Research Ed.). 349: g6154. doi:10.1136/bmj.g6154. PMID 25341679.
- GBD 2015 Disease and Injury Incidence and Prevalence, Collaborators. (8 October 2016). "Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990-2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1545–1602. doi:10.1016/S0140-6736(16)31678-6. PMC 5055577. PMID 27733282.
- GBD 2015 Mortality and Causes of Death, Collaborators. (8 October 2016). "Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1459–1544. doi:10.1016/s0140-6736(16)31012-1. PMC 5388903. PMID 27733281.
- "Hernia". www.nlm.nih.gov. 9 August 2014. Archived from the original on 16 March 2015. Retrieved 12 March 2015.
- Nigam, VK (2009). Essentials of Abdominal Wall Hernias. I. K. International Pvt Ltd. p. 6. ISBN 9788189866938. Archived from the original on 2017-09-08.
- "Symptoms". Archived from the original on 2010-02-13. Retrieved 2010-05-24.
- Lee HK, Park SJ, Yi BH (2010). "Multidetector CT reveals diverse variety of abdominal hernias". Diagnostic Imaging. 32 (5): 27–31. Archived from the original on 2010-06-18.
- Trudie A Goers; Washington University School of Medicine Department of Surgery; Klingensmith, Mary E; Li Ern Chen; Sean C Glasgow (2008). The Washington manual of surgery. Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins. ISBN 978-0-7817-7447-5.CS1 maint: multiple names: authors list (link)
- onlinedictionary.datasegment.com > incarcerated Archived 2008-11-20 at the Wayback Machine Citing: Webster 1913
- "Hiatal Hernia Symptoms, Causes And Relation To Acid Reflux And Heartburn". Archived from the original on October 28, 2008. Retrieved 2010-05-24.
- "Hernia Causes". Archived from the original on 2010-05-31. Retrieved 2010-05-24.
- Desarda MP (2003). "Surgical physiology of inguinal hernia repair—a study of 200 cases". BMC Surg. 3: 2. doi:10.1186/1471-2482-3-2. PMC 155644. PMID 12697071.
- Jones, Riley (2013). "An unexpected finding during an inguinal herniorrhaphy: report of an indirect hernia with two hernia sacs". Journal of Pediatric Surgery Case Reports. 1 (10): 331–332. doi:10.1016/j.epsc.2013.09.002.
- Bosanquet, DC; Ansell, J; Abdelrahman, T; Cornish, J; Harries, R; Stimpson, A; Davies, L; Glasbey, JC; Frewer, KA; Frewer, NC; Russell, D; Russell, I; Torkington, J (2015). "Systematic Review and Meta-Regression of Factors Affecting Midline Incisional Hernia Rates: Analysis of 14,618 Patients". PLOS ONE. 10 (9): e0138745. doi:10.1371/journal.pone.0138745. PMC 4577082. PMID 26389785.
- Arráez-Aybar, L. A., González-Gómez, C. C., & Torres-García, A. J. (2009). Morgagni-Larrey parasternal diaphragmatic hernia in the adult. Rev Esp Enferm Dig, 101(5), 357-366.
- "Archived copy". Archived from the original on 2017-07-14. Retrieved 2017-07-23.CS1 maint: archived copy as title (link)
- Effectiveness of mesh hernioplasty in incarcerated inguinal hernias. Kamtoh G, Pach R, Kibil W, Matyja A, Solecki R, Banas B, Kulig J. 2014 Sep;9(3):415-9. doi:10.5114/wiitm.2014.43080
- Sohail MR, Smilack JD (June 2004). "Hernia repair mesh-associated Mycobacterium goodii infection". J. Clin. Microbiol. 42 (6): 2858–60. doi:10.1128/JCM.42.6.2858-2860.2004. PMC 427896. PMID 15184492.
- Global Burden of Disease Study 2013, Collaborators (22 August 2015). "Global, regional, and national incidence, prevalence, and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013". Lancet. 386 (9995): 743–800. doi:10.1016/s0140-6736(15)60692-4. PMC 4561509. PMID 26063472.
- GBD 2013 Mortality and Causes of Death, Collaborators (17 December 2014). "Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013". Lancet. 385 (9963): 117–71. doi:10.1016/S0140-6736(14)61682-2. PMC 4340604. PMID 25530442.
External links
| Classification | |
|---|---|
| External resources |
| Look up hernia in Wiktionary, the free dictionary. |
| Wikimedia Commons has media related to Hernias. |
- Hernia at Curlie