Intensive care medicine
Intensive care medicine, or critical care medicine, is a branch of medicine concerned with the diagnosis and management of life-threatening conditions that may require sophisticated life support and intensive monitoring.

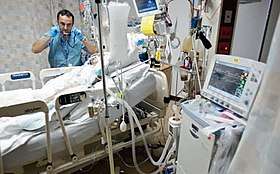 Example patient managed under intensive care | |
| Significant diseases | Respiratory failure, Organ failure, Multiorgan failure |
|---|---|
| Specialist | Intensivist |
Overview
Patients requiring intensive care may require support for different forms of shock, which include but are not limited to, cardiovascular instability (hypertension/hypotension), sepsis, and potentially lethal cardiac arrhythmias.[1] Other causes include airway or respiratory compromise (such as ventilator support), acute renal failure, or the cumulative effects of multiple organ failure, more commonly referred to now as multiple organ dysfunction syndrome.[1] They may also be admitted for intensive/invasive monitoring, such as the crucial hours after major surgery when deemed too unstable to transfer to a less intensively monitored unit.[2]
Patient management in intensive care differs between countries. Closed or Open ICUs structures may be used for care of patients.[2] In a closed unit, the intensive care specialist takes on the senior role for all patients in the unit.[2] Some countries have open ICUs, where the primary physician chooses to admit and, patient care is coordinated by multiple general physician which may or may not include an intensivist.[2][3] There is increasingly strong evidence that "closed" intensive care units staffed by intensivists provide better outcomes for patients.[4][5] Open structure is the most common in the United States but the closed structure is often found at US large academic centers.[2] Intermediate structures that fall somewhere in between an open or closed ICU structure also exist.[2]
Organization of Treatment
Intensive care usually takes a system-by-system approach to treatment. As such, the nine key systems are each considered on an observation-intervention-impression basis to produce a daily plan. In addition to the key systems, intensive care treatment raises other issues including psychological health, pressure points, mobilization and physiotherapy, and secondary infections.
In alphabetical order, the nine key systems considered in the intensive care setting are: cardiovascular system, central nervous system, endocrine system, gastro-intestinal tract (and nutritional condition), hematology, integumentary system, microbiology (including sepsis status), renal (and metabolic), and respiratory system.
Intensive Care Unit Types
Intensive care is usually provided in a specialized unit of a hospital called the intensive care unit (ICU) or critical care unit (CCU). Many hospitals also have designated intensive care areas for certain specialties of medicine, such as the coronary intensive care unit (CCU or sometimes CICU) for heart disease, medical intensive care unit (MICU), surgical intensive care unit (SICU), pediatric intensive care unit (PICU), neuroscience critical care unit (NCCU), overnight intensive-recovery (OIR), shock/trauma intensive-care unit (STICU), neonatal intensive care unit (NICU), and other units as dictated by the needs and available resources of each hospital. The naming is not rigidly standardized. For a time in the early 1960s, it was not clear that specialized intensive care units were needed, so intensive care resources were brought to the room of the patient that needed the additional monitoring, care, and resources. It became rapidly evident, however, that a fixed location where intensive care resources and dedicated personnel were available provided better care than ad hoc provision of intensive care services spread throughout a hospital.
Common Equipment
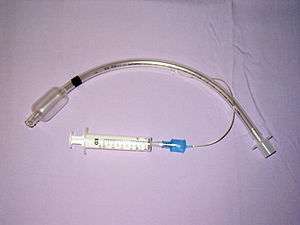
A number of these devices may be used in intensive care medicine, though some of these can also be used outside of the ICU and even outside of the hospital.
Equipment
- Common equipment in an intensive care unit includes:
- Mechanical ventilation to assist breathing through an endotracheal tube or a tracheotomy
- Hemofiltration equipment for acute kidney injury
- Monitoring equipment
- Intravenous lines
- Nasogastric tubes, suction pumps, drains and catheters
Drugs
A wide array of drugs including but not limited to: inotropes, sedatives, broad spectrum antibiotics and analgesics.
Common Procedures
Central line placement - for drug infusions, fluids or total parenteral nutrition
Echocardiogram - Evaluate function and structure of the heart
Bronchoscopy - Provides a way to look at lungs and air ways, may also allow physicians to obtain a sample of fluid within the lungs
Ultrasound - Allows health care providers to evaluate internal structures
Paracentesis - Diagnostic and therapeutic. Removal of fluid from abdominal cavity.
Medical specialties
ICU care requires more specialized patient care; this need has led to the use of a multidisciplinary team to provide care for patients.[1] Staffing between Intensive care units by country, hospital, unit, or institution.[2]
Physician
Critical care medicine is an increasingly important medical specialty. Physicians with training in critical care medicine are referred to as intensivists.[6] In the United States, the specialty requires additional fellowship training for physicians having completed their primary residency training in internal medicine, pediatrics, anesthesiology, surgery or emergency medicine. US board certification in critical care medicine is available through all five specialty boards. Intensivists with a primary training in internal medicine sometimes pursue combined fellowship training in another subspecialty such as pulmonary medicine, cardiology, infectious disease, or nephrology. The American Society of Critical Care Medicine is a well-established multiprofessional society for practitioners working in the ICU including nurses, respiratory therapists, and physicians. Most medical research has demonstrated that ICU care provided by intensivists produces better outcomes and more cost-effective care.[7] This has led the Leapfrog Group to make a primary recommendation that all ICU patients be managed or co-managed by a dedicated intensivist who is exclusively responsible for patients in one ICU.
Nursing
Nurses that work in the critical care setting are typically registered nurses.[8] Nurses may pursue additional education and training in critical care medicine leading to certification as a CCRN by the American Association of Critical Care Nurses a standard that was begun in 1975.[9] These certifications became more specialized to the patient population in 1997 by the American Association of Critical care Nurses, to include pediatrics, neonatal and adult.[9]
Nurse Practitioners and Physician Assistants
Nurse Practitioners and Physician Assistants are another type of non-physician provider that care for patients in ICUs.[1] Outcomes have shown that the use of non-physician providers have been shown to have similar outcomes to those with physician providers.[2] These providers have less years of in school training and typically receive further clinical on the job education.[2] Non-physician providers like nurse practitioners and physician assistants are typically present for longer periods of time than resident physicians that rotate off service.[2]
Pharmacist
Critical care Pharmacists work with the medical team in many aspect but some include, monitoring serum concentrations of medication, past medication use, current medication use, and medication allergies.[3] Their typically round with the team but it may differ by institution.[3] Some pharmacist after attaining their doctorate or pharmacy may pursue additional training in a postgraduate residency and become certified as critical care pharmacists.[3] Pharmacists help manage all aspects of drug therapy and may pursue additional credentialing in critical care medicine as BCCCP by the Board of Pharmaceutical Specialties. Many critical care pharmacist are a part of the multi-professional Society of Critical Care Medicine.[3] Inclusion of pharmacist decreases drug reactions and poor outcomes for patients.[1]
Paramedics or Emergency medical Technicians
Paramedics are certified to levels of CCEMT-P, PNCCT-P, CCP-C and/or FP-C depending upon their speciality (e.g. air, ground, adult, pediatric and/or neonatal medicine).
Registered dietitian
Nutrition in the intensive care unit presents unique challenges due to changes in patient metabolism and physiology while critically ill.[10] Critical care nutrition is rapidly becoming a subspecialty for dieticians who can pursue additional training and achieve certification in enteral and parenteral nutrition through the American Society for Parenteral and Enteral Nutrition (ASPEN).
Respiratory therapist
Respiratory therapist often work in Intensive Care units to monitor how well a patient is breathing.[11] Respiratory therapists may pursue additional education and training leading to credentialing in adult critical care (ACCS) and neonatal and pediatric (NPS) specialties.These therapist have been trained to monitor a patient's breathing, provide treatments to help their breathing and evaluate for improvement.[11] They may be involved in emergency care like managing an airway, humidification of oxygen, administering diagnostic test, and providing physiotherapy.[12]
Other Considerations
Medical studies suggest a relation between ICU volume and quality of care for mechanically ventilated patients.[13] After adjustment for severity of illness, demographic variables, and characteristics of the ICUs (including staffing by intensivists), higher ICU volume was significantly associated with lower ICU and hospital mortality rates. For example, adjusted ICU mortality (for a patient at average predicted risk for ICU death) was 21.2% in hospitals with 87 to 150 mechanically ventilated patients annually, and 14.5% in hospitals with 401 to 617 mechanically ventilated patients annually. Hospitals with intermediate numbers of patients had outcomes between these extremes. ICU delirium, formerly and inaccurately referred to as ICU psychosis, is a syndrome common in intensive care and cardiac units where patients who are in unfamiliar, monotonous surroundings develop symptoms of delirium (Maxmen & Ward, 1995). This may include interpreting machine noises as human voices, seeing walls quiver, or hallucinating that someone is tapping them on the shoulder.[14] There exists systematic reviews in which interventions of sleep promotion related outcomes in the ICU have proven impactful in the overall health of patients in the ICU.[15]
Intensive Care Medicine Economics
In general, it is the most expensive, technologically advanced and resource-intensive area of medical care. In the United States, estimates of the 2000 expenditure for critical care medicine ranged from US$19–55 billion. During that year, critical care medicine accounted for 0.56% of GDP, 4.2% of national health expenditure and about 13% of hospital costs.[16] In 2011, hospital stays with ICU services accounted for just over one-quarter of all discharges (29.9%) but nearly one-half of aggregate total hospital charges (47.5%) in the United States. The mean hospital charge was 2.5 times higher for discharges with ICU services than for those without.[17]
History
Florence Nightingale era

The ICU's roots can be traced back to the Monitoring Unit of critical patients through nurse Florence Nightingale. The Crimean War began in 1853 when Britain, France, and the Ottoman Empire (Turkey) declared war on Russia. Because of the lack of critical care and the high rate of infection, there was a high mortality rate of hospitalised soldiers, reaching as high as 40% of the deaths recorded during the war. Upon Nightingale's arrival and practicing, the mortality rate fell to 2%. Nightingale contracted typhoid, and returned in 1856 from the war. A school of nursing dedicated to her was formed in 1859 in England. The school was recognised for its professional value and technical calibre, receiving prizes throughout the British government. The school of nursing was established in Saint Thomas Hospital, as a one-year course, and was given to doctors. It used theoretical and practical lessons, as opposed to purely academic lessons. Nightingale's work, and the school, paved the way for intensive care medicine.
Dandy era
Walter Edward Dandy was born in Sedalia, Missouri. He received his BA in 1907 through the University of Missouri and his M.D. in 1910 through the Johns Hopkins School of Medicine. Dandy worked one year with Dr. Harvey Cushing (the father of modern neurosurgery) in the Hunterian Laboratory of Johns Hopkins before entering its boarding school and residence in the Johns Hopkins Hospital. He worked at Johns Hopkins University in 1914 and remained there until his death in 1946. One of the most important contributions he made for neurosurgery was the air method in ventriculography, in which the cerebrospinal fluid is substituted with air to help an image form on an X-ray of the ventricular space in the brain. This technique was extremely successful for identifying brain injuries. Dr. Dandy was also a pioneer in the advances in operations for illnesses of the brain affecting the glossopharyngeal nerve as well as Ménière's syndrome, and he published studies that show that high activity can cause sciatic pain. Walker Dandy, famed John's Hopkins neurosurgeon is noted to have created a special unit in 1923 for critically ill patients. [18]
Ibsen era
Bjørn Aage Ibsen (1915–2007) graduated in 1940 from medical school at the University of Copenhagen and trained in anesthesiology from 1949 to 1950 at the Massachusetts General Hospital, Boston. He became involved in the 1952 poliomyelitis outbreak in Denmark,[19] where 2722 patients developed the illness in a 6-month period, with 316 suffering respiratory or airway paralysis. Treatment had involved the use of the few negative pressure respirators available, but these devices, while helpful, were limited and did not protect against aspiration of secretions. Ibsen changed management directly, instituting protracted positive pressure ventilation by means of intubation into the trachea, and enlisting 200 medical students to manually pump oxygen and air into the patients' lungs.[20] At this time Carl-Gunnar Engström had developed one of the first positive pressure volume controlled ventilators, which eventually replaced the medical students. In this fashion, mortality declined from 90% to around 25%. Patients were managed in three special 35-bed areas, which aided charting and other management. In 1953, Ibsen set up what became the world's first Medical/Surgical ICU in a converted student nurse classroom in Kommunehospitalet (The Municipal Hospital) in Copenhagen,[19] and provided one of the first accounts of the management of tetanus with muscle relaxants and controlled ventilation. In 1954 Ibsen was elected Head of the Department of Anaesthesiology at that institution. He jointly authored the first known account of ICU management principles in Nordisk Medicin, 18 September 1958: ‘Arbejdet på en Anæsthesiologisk Observationsafdeling’ (‘The Work in an Anaesthesiologic Observation Unit’) with Tone Dahl Kvittingen from Norway. He died in 2007.
Safar era
The first surgical ICU was established in Baltimore. In 1962, in the University of Pittsburgh, the first Critical Care Residency was established in the United States.
In 1970, the Society of Critical Care Medicine was formed.[21]
See also
Notes
- Basics of anesthesia. Pardo, Manuel, Jr., 1965-, Miller, Ronald D., 1939-, Preceded by (work): Miller, Ronald D., 1939- (Seventh edition ed.). Philadelphia, PA. ISBN 9780323401159. OCLC 989157369.CS1 maint: others (link) CS1 maint: extra text (link)
- Principles of critical care. Hall, Jesse B.,, Schmidt, Gregory A.,, Kress, John P., (Fourth edition ed.). New York. ISBN 9780071738811. OCLC 906700899.CS1 maint: extra punctuation (link) CS1 maint: others (link) CS1 maint: extra text (link)
- Evidence-based practice of critical care. Deutschman, Clifford S.,, Neligan, Patrick J., (Third edition ed.). Philadelphia, PA. ISBN 978-0-323-64069-5. OCLC 1118693260.CS1 maint: extra punctuation (link) CS1 maint: others (link) CS1 maint: extra text (link)
- Manthous, CA; Amoateng-Adjepong, Y; Al-Kharrat, T; Jacob, B; Alnuaimat, HM; Chatila, W; Hall, JB (1997). "Effects of a medical intensivist on patient care in a community teaching hospital". Mayo Clinic Proceedings (Abstract). 72 (5): 391–9. doi:10.4065/72.5.391. PMID 9146680.
- Hanson CW; Deutschman, CS; Anderson, HL; Reilly, PM; Behringer, EC; Schwab, CW; Price, J (1999). "Effects of an organized critical care service on outcomes and resource utilization: a cohort study". Critical Care Medicine (Abstract). 27 (2): 270–4. doi:10.1097/00003246-199902000-00030. PMID 10075049.
- "What – or Who -- Is an Intensivist?". Healthcare Financial Management Association. Archived from the original on 27 September 2009.
- "Association between Critical Care Physician Management and Patient Mortality in the Intensive Care Unit". Annals of Internal Medicine. 3 June 2008. Volume 148, Issue 11. pp. 801–809.
- Principles of critical care. Hall, Jesse B.,, Schmidt, Gregory A.,, Kress, John P., (Fourth edition ed.). New York. ISBN 9780071738811. OCLC 906700899.CS1 maint: extra punctuation (link) CS1 maint: others (link) CS1 maint: extra text (link)
- Pediatric critical care. Fuhrman, Bradley P.,, Zimmerman, Jerry J.,, Clark, Robert S. B., 1962-, Relvas, Monica S.,, Thompson, Ann E.,, Tobias, Joseph D., (Fifth edition ed.). Philadelphia, PA. ISBN 978-0-323-37839-0. OCLC 966447977.CS1 maint: extra punctuation (link) CS1 maint: others (link) CS1 maint: extra text (link)
- Current surgical therapy. Cameron, John L.,, Cameron, Andrew M. (Andrew MacGregor), (12th edition ed.). Philadelphia, PA. ISBN 978-0-323-37691-4. OCLC 966447396.CS1 maint: extra punctuation (link) CS1 maint: others (link) CS1 maint: extra text (link)
- Total burn care. Herndon, David N., (Fifth edition ed.). Edinburgh. ISBN 978-0-323-49742-8. OCLC 1012122839.CS1 maint: extra punctuation (link) CS1 maint: others (link) CS1 maint: extra text (link)
- Gomella, Leonard G. (2007). Clinician's pocket reference. Haist, Steven A., University of Kentucky. College of Medicine. (11th ed ed.). New York: McGraw-Hill Companies, Inc. ISBN 0-07-145428-4. OCLC 85841308.CS1 maint: extra text (link)
- Kahn, JM; Goss, CH; Heagerty, PJ; Kramer, AA; O'Brien, CR; Rubenfeld, GD (2006). "Hospital volume and the outcomes of mechanical ventilation". The New England Journal of Medicine. 355 (1): 41–50. doi:10.1056/NEJMsa053993. PMID 16822995.
- Nolen-Hoeksema, Susan. "Neurodevelopmental and Neurocognitive Disorders." (Ab)normal Psychology. Sixth ed. New York City: McGraw-Hill Education, 2014. 314. Print.
- Flannery, Alexander H.; Oyler, Douglas R.; Weinhouse, Gerald L. (December 2016). "The Impact of Interventions to Improve Sleep on Delirium in the ICU". Critical Care Medicine. 44 (12): 2231–2240. doi:10.1097/ccm.0000000000001952. ISSN 0090-3493. PMID 27509391.
- Halpern, Neil A.; Pastores, Stephen M.; Greenstein, Robert J. (June 2004). "Critical care medicine in the United States 1985–2000: An analysis of bed numbers, use, and costs". Critical Care Medicine. 32 (6): 1254–1259. doi:10.1097/01.CCM.0000128577.31689.4C. PMID 15187502.
- Barrett ML; Smith MW; Elizhauser A; Honigman LS; Pines JM (December 2014). "Utilization of Intensive Care Services, 2011". HCUP Statistical Brief #185. Rockville, MD: Agency for Healthcare Research and Quality.
- Miller's anesthesia. Gropper, Michael A., 1958-, Miller, Ronald D., 1939- (Ninth edition ed.). Philadelphia, PA. ISBN 978-0-323-61264-7. OCLC 1124935549.CS1 maint: others (link) CS1 maint: extra text (link)
- "The Danish anaesthesiologist Björn Ibsen a pioneer of long-term ventilation on the upper airways, Louise Reisner-Sénélar, 2009" (pdf).
- Reisner-Sénélar, Louise (2011). "The Birth of Intensive Care Medicine: Björn Ibsen’s Records" (PDF format).Intensive Care Medicine. Retrieved 2 October 2012.
- history reference: Brazilian Society of Critical Care SOBRATI Video:ICU History Historical photos
References
- Intensive Care Medicine by Irwin and Rippe
- Civetta, Taylor, and Kirby's Critical Care
- The ICU Book by Marino
- Procedures and Techniques in Intensive Care Medicine by Irwin and Rippe
- Halpern NA, Pastores SM, Greenstein RJ (June 2004). "Critical care medicine in the United States 1985–2000: an analysis of bed numbers, use, and costs". Critical Care Medicine. 32 (6): 1254–9. doi:10.1097/01.CCM.0000128577.31689.4C. PMID 15187502..
- History references:
- Society of Critical Care Medicine
- Reynolds, H.N.; Rogove, H.; Bander, J.; McCambridge, M.; et al. (December 2011). "A working lexicon for the tele-intensive care unit: We need to define tele-intensive care unit to grow and understand it" (PDF). Telemedicine and E-Health. 17 (10): 773–783. doi:10.1089/tmj.2011.0045. hdl:2027.42/90470. PMID 22029748.
- Olson, Terrah; Brasel, Karen; Redmann, Andrew; Alexander, G.; Schwarze, Margaret (January 2013). "Surgeon-Reported Conflict With Intensivists About Postoperative Goals of Care". JAMA Surgery. 148 (1): 29–35. doi:10.1001/jamasurgery.2013.403. PMC 3624604. PMID 23324837.
Further reading
- Lois Reynolds; Tilli Tansey, eds. (2011), History of British Intensive Care, c. 1950–c. 2000, Wellcome Witnesses to Contemporary Medicine, History of Modern Biomedicine Research Group, ISBN 978-0-902238-75-6, Wikidata Q29581786.
External links
| Wikimedia Commons has media related to Intensive-care medicine. |
| Wikibooks has a book on the topic of: Intensive Care Medicine |
- College of Intensive Care Medicine - Australia and New Zealand
- Australia and New Zealand Intensive Care Society
- Society of Critical Care Medicine
- Veterinary Emergency And Critical Care Society
- ESICM: European Society of Intensive Care Medicine
- ESPNIC: The society for paediatric and neonatal intensive care healthcare professionals in Europe
- UK Intensive Care Society
- Scottish Intensive Care Society
- Hong Kong Society of Critical Care Medicine
- Chinese Society of Critical Care Medicine
- Taiwan Society of Critical Care Medicine
- From Iron Lungs to Intensive Care, Royal Institution debate, February 2012