Auricular branch of vagus nerve
The auricular branch of the vagus nerve is often termed the Alderman's nerve or Arnold's nerve. The latter name is an eponym for Friedrich Arnold.[1] The auricular branch of the vagus nerve supplies sensory innervation to the skin of the ear canal, tragus, and auricle.
| Auricular branch of vagus nerve | |
|---|---|
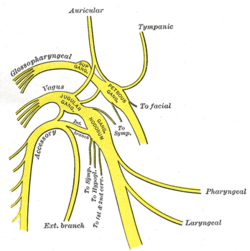 Plan of upper portions of glossopharyngeal, vagus, and accessory nerves (auricular labeled at top center) | |
| Details | |
| From | vagus nerve |
| Identifiers | |
| Latin | Ramus auricularis nervi vagi |
| TA | A14.2.01.156 |
| FMA | 6232 |
| Anatomical terms of neuroanatomy | |
Path
It arises from the superior ganglion of the vagus nerve, and is joined soon after its origin by a filament from the petrous ganglion of the glossopharyngeal; it passes behind the internal jugular vein, and enters the mastoid canaliculus on the lateral wall of the jugular fossa.
Traversing the substance of the temporal bone, it crosses the facial canal about 4 mm (0.16 in) above the stylomastoid foramen, and here it gives off an ascending branch which joins the facial nerve.
The nerve reaches the surface by passing through the tympanomastoid fissure between the mastoid process and the tympanic part of the temporal bone, and divides into two branches:
- one joins the posterior auricular nerve.
- the other is distributed to the skin of the back of the ear (auricle) and to the posterior part of the ear canal.
Clinical significance
This nerve may be involved by the glomus jugulare tumour.
Laryngeal cancer can present with pain behind the ear and in the ear - this is a referred pain through the vagus nerve to the nerve of Arnold.
In a small portion of individuals, the auricular nerve is the afferent limb of the Ear-Cough or Arnold Reflex.[2] Physical stimulation of the external acoustic meatus innervated by the auricular nerve elicits a cough, much like the other cough reflexes associated with the vagus nerve. Rarely, on introduction of speculum in the external ear, patients have experienced syncope due to the stimulation of the auricular branch of the vagus nerve.
Clinical application
This nerve may be stimulated as a diagnostic or therapeutic technique
Transcutaneous vagus nerve stimulation (tVNS) was proposed by Ventureya (2000) for seizures.[3] In 2003 Fallgatter et al. published "Far field potentials from the brain stem after transcutaneous vagus nerve stimulation"[4] and in 2007 Kraus et al. did the first tVNS-fMRI study.[5] In Europe, a device was approved for seizure treatment (NEMOS by CerboMed). Although the transcutaneous method has not been specifically approved in the United States (i.e. off-label) it is legal and being investigated (and found to be effective and safe) for many conditions including:
References
This article incorporates text in the public domain from page 911 of the 20th edition of Gray's Anatomy (1918)
- synd/258 at Who Named It?
- Brendan J. Canning, PhD (January 2006). "Anatomy and Neurophysiology of the Cough Reflex". CHEST. Retrieved 2009-03-09.
- Ventureyra EC. (February 2000). "Transcutaneous vagus nerve stimulation for partial onset seizure therapy. A new concept". Childs Nerv Syst. 16 (2): 101–2. doi:10.1007/s003810050021. PMID 10663816.
- Fallgatter AJ, Neuhauser B, Herrmann MJ, Ehlis AC, Wagener A, Scheuerpflug P, Reiners K, Riederer P (December 2003). "Far field potentials from the brain stem after transcutaneous vagus nerve stimulation". Childs Nerv Syst. 110 (12): 1437–43. doi:10.1007/s00702-003-0087-6. PMID 14666414.
- Kraus T, Hösl K, Kiess O, Schanze A, Kornhuber J, Forster C (2007). "BOLD fMRI deactivation of limbic and temporal brain structures and mood enhancing effect by transcutaneous vagus nerve stimulation". J Neural Transm (Vienna). 114 (11): 1485–93. doi:10.1007/s00702-007-0755-z. PMID 17564758.
- Stavrakis S, Humphrey MB, Scherlag BJ, Hu Y, Jackman WM, Nakagawa H, Lockwood D, Lazzara R, Po SS (Mar 2015). "Low-level transcutaneous electrical vagus nerve stimulation suppresses atrial fibrillation". J Am Coll Cardiol. 65 (9): 867–75. doi:10.1016/j.jacc.2014.12.026. PMC 4352201. PMID 25744003.
- Yu L, Scherlag BJ, Li S, Fan Y, Dyer J, Male S, Varma V, Sha Y, Stavrakis S, Po SS (March 2013). "Low-level transcutaneous electrical stimulation of the auricular branch of the vagus nerve: a noninvasive approach to treat the initial phase of atrial fibrillation". Heart Rhythm. 10 (3): 428–35. doi:10.1016/j.hrthm.2012.11.019. PMID 23183191.
- Hein E, Nowak M, Kiess O, Biermann T, Bayerlein K, Kornhuber J, Kraus T (May 2013). "Auricular transcutaneous electrical nerve stimulation in depressed patients: a randomized controlled pilot study". J Neural Transm (Vienna). 120 (5): 821–7. doi:10.1007/s00702-012-0908-6. PMID 23117749.
- Aaronson ST, Carpenter LL, Conway CR, Reimherr FW, Lisanby SH, Schwartz TL, Moreno FA, Dunner DL, Lesem MD, Thompson PM, Husain M, Vine CJ, Banov MD, Bernstein LP, Lehman RB, Brannon GE, Keepers GA, O'Reardon JP, Rudolph RL, Bunker M (July 2013). "Vagus nerve stimulation therapy randomized to different amounts of electrical charge for treatment-resistant depression: acute and chronic effects". Brain Stimul. 6 (4): 631–40. doi:10.1016/j.brs.2012.09.013. PMID 23122916.
- Huang F, Dong J, Kong J, Wang H, Meng H, Spaeth RB, Camhi S, Liao X, Li X, Zhai X, Li S, Zhu B, Rong P (June 2014). "Effect of transcutaneous auricular vagus nerve stimulation on impaired glucose tolerance: a pilot randomized study". BMC Complement Altern Med. 14: 203. doi:10.1186/1472-6882-14-203. PMC 4227038. PMID 24968966.
- Huston JM, Gallowitsch-Puerta M, Ochani M, Ochani K, Yuan R, Rosas-Ballina M, Ashok M, Goldstein RS, Chavan S, Pavlov VA, Metz CN, Yang H, Czura CJ, Wang H, Tracey KJ (December 2007). "Transcutaneous vagus nerve stimulation reduces serum high mobility group box 1 levels and improves survival in murine sepsis". Crit. Care Med. 35 (12): 2762–8. doi:10.1097/01.CCM.0000288102.15975.BA. PMID 17901837.
- Jacobs HI, Riphagen JM, Razat CM, Wiese S, Sack AT (May 2015). "Transcutaneous vagus nerve stimulation boosts associative memory in older individuals". Neurobiol Aging. 36 (5): 1860–7. doi:10.1016/j.neurobiolaging.2015.02.023. PMID 25805212.
- Wang Z, Zhou X, Sheng X, Yu L, Jiang H (2015). "Unilateral low-level transcutaneous electrical vagus nerve stimulation: A novel noninvasive treatment for myocardial infarction". Int J Cardiol. 190: 9–10. doi:10.1016/j.ijcard.2015.04.087. PMID 25912108.
- Kreuzer PM, Landgrebe M, Resch M, Husser O, Schecklmann M, Geisreiter F, Poeppl TB, Prasser SJ, Hajak G, Rupprecht R, Langguth B (September 2014). "Feasibility, safety and efficacy of transcutaneous vagus nerve stimulation in chronic tinnitus: an open pilot study". Brain Stimul. 7 (5): 740–7. doi:10.1016/j.brs.2014.05.003. PMID 24996510.
- Cai PY, Bodhit A, Derequito R, Ansari S, Abukhalil F, Thenkabail S, Ganji S, Saravanapavan P, Shekar CC, Bidari S, Waters MF, Hedna VS (June 2014). "Vagus nerve stimulation in ischemic stroke: old wine in a new bottle". Front. Neurol. 5: 107. doi:10.3389/fneur.2014.00107. PMC 4067569. PMID 25009531.