Hyperprolactinaemia
Hyperprolactinaemia is the presence of abnormally high levels of prolactin in the blood. Normal levels are less than 500 mIU/L [23.5 ng/mL or μg/L] for women, and less than 450 mI U/L [21.5 ng/mL or μg/L] for men .
| Hyperprolactinemia | |
|---|---|
| Other names | Hyperprolactinemia |
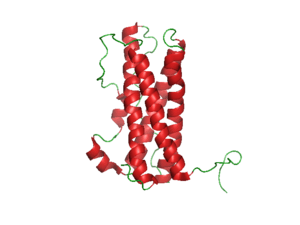 | |
| Prolactin | |
| Specialty | Endocrinology |
Prolactin is a peptide hormone produced by the anterior pituitary gland that is primarily associated with lactation and plays a vital role in breast development during pregnancy. Hyperprolactinaemia may cause galactorrhea (production and spontaneous flow of breast milk), infertility, and disruptions in the normal menstrual period in women; and hypogonadism, infertility and erectile dysfunction in men.
Hyperprolactinaemia can also be a part of normal body changes during pregnancy and breastfeeding. It can also be caused by diseases affecting the hypothalamus and pituitary gland. It can also be caused by disruption of the normal regulation of prolactin levels by drugs, medicinal herbs and heavy metals inside the body. Hyperprolactinaemia may also be the result of disease of other organs such as the liver, kidneys, ovaries and thyroid.[1]
Signs and symptoms
In women, a high blood level of prolactin often causes hypoestrogenism with anovulatory infertility and a decrease in menstruation. In some women, menstruation may disappear altogether (amenorrhoea). In others, menstruation may become irregular or menstrual flow may change. Women who are not pregnant or nursing may begin producing breast milk. Some women may experience a loss of libido (interest in sex) and breast pain, especially when prolactin levels begin to rise for the first time, as the hormone promotes tissue changes in the breast. Intercourse may become difficult or painful because of vaginal dryness.
In men, the most common symptoms of hyperprolactinaemia are decreased libido, sexual dysfunction (in both men and women), erectile dysfunction, infertility, and gynecomastia. Because men have no reliable indicator such as menstruation to signal a problem, many men with hyperprolactinaemia being caused by a pituitary adenoma may delay going to the doctor until they have headaches or eye problems caused by the enlarged pituitary pressing against the adjacent optic chiasm. They may not recognize a gradual loss of sexual function or libido. Only after treatment do some men realize they had a problem with sexual function.
Because of hypoestrogenism and hypoandrogenism, hyperprolactinaemia can lead to osteoporosis.
Causes
Hyperprolactinaemia may be caused by either disinhibition (e.g., compression of the pituitary stalk or reduced dopamine levels) or excess production from a prolactinoma (a type of pituitary adenoma). A blood serum prolactin level of 1000–5000 mIU/L could be from either mechanism, but >5000 mIU/L (>200 μg/L) is likely due to the activity of an adenoma; macroadenomas (large tumours over 10 mm diameter) have levels of prolactin up to 100,000 mIU/L.
Hyperprolactinemia inhibits the secretion of gonadotropin-releasing hormone (GnRH) from the hypothalamus, which in turn inhibits the release of follicle-stimulating hormone (FSH) and luteinizing hormone (LH) from the pituitary gland and results in diminished gonadal sex hormone production (termed hypogonadism).[2] This is the cause of many of the symptoms described below.
In many people, elevated prolactin levels remain unexplained and may represent a form of hypothalamic–pituitary–adrenal axis dysregulation.
| Causes of hyperprolactinemia[3] | |
|---|---|
| Physiologic hypersecretion | |
| Hypothalamic-pituitary stalk damage |
|
| Pituitary hypersecretion | |
| Systemic disorders | |
| Drug-induced hypersecretion |
Physiological causes
Physiological (i.e., non-pathological) causes include: pregnancy, breastfeeding, and mental stress.
Medications
Prolactin secretion in the pituitary is normally suppressed by the brain chemical dopamine. Drugs that block the effects of dopamine at the pituitary or deplete dopamine stores in the brain may cause the pituitary to secrete prolactin. These drugs include the typical antipsychotics: phenothiazines such as chlorpromazine (Thorazine), and butyrophenones such as haloperidol (Haldol); atypical antipsychotics such as risperidone (Risperdal) and paliperidone (Invega);[4][5] gastroprokinetic drugs used to treat gastro-oesophageal reflux and medication-induced nausea (such as that from chemotherapy): metoclopramide (Reglan) and domperidone; less often, alpha-methyldopa and reserpine, used to control hypertension; and also estrogens and TRH.[4][6] The sleep drug ramelteon (Rozerem) also increases the risk of hyperprolactinaemia. A benzodiazepine analog, etizolam, can also increase the risk of hyperprolactinaemia. In particular, the dopamine antagonists metoclopramide and domperidone are both powerful prolactin stimulators and have been used to stimulate breast milk secretion for decades. However, since prolactin is antagonized by dopamine and the body depends on the two being in balance, the risk of prolactin stimulation is generally present with all drugs that deplete dopamine, either directly or as a rebound effect.
Specific diseases
Prolactinoma or other tumours arising in or near the pituitary — such as those that cause acromegaly may block the flow of dopamine from the brain to the prolactin-secreting cells, likewise, division of the pituitary stalk or hypothalamic disease. Other causes include chronic kidney failure, hypothyroidism, bronchogenic carcinoma and sarcoidosis. Some women with polycystic ovary syndrome may have mildly-elevated prolactin levels.
Nonpuerperal mastitis may induce transient hyperprolactinemia (neurogenic hyperprolactinemia) of about three weeks' duration; conversely, hyperprolactinemia may contribute to nonpuerperal mastitis.[7]
Apart from diagnosing hyperprolactinaemia and hypopituitarism, prolactin levels are often checked by physicians in patients that have suffered a seizure, when there is doubt as to whether they have had an epileptic seizure or a non-epileptic seizure. Shortly after epileptic seizures, prolactin levels often rise, whereas they are normal in non-epileptic seizures.
Diagnosis
A doctor will test for prolactin blood levels in women with unexplained milk secretion (galactorrhea) or irregular menses or infertility, and in men with impaired sexual function and milk secretion. If prolactin is high, a doctor will test thyroid function and ask first about other conditions and medications known to raise prolactin secretion. While a plain X-ray of the bones surrounding the pituitary may reveal the presence of a large macro-adenoma, the small micro-adenoma will not be apparent. Magnetic resonance imaging (MRI) is the most sensitive test for detecting pituitary tumours and determining their size. MRI scans may be repeated periodically to assess tumour progression and the effects of therapy. Computed Tomography (CT scan) also gives an image of the pituitary, but it is less sensitive than the MRI.
In addition to assessing the size of the pituitary tumour, doctors also look for damage to surrounding tissues, and perform tests to assess whether production of other pituitary hormones is normal. Depending on the size of the tumour, the doctor may request an eye exam with measurement of visual fields.
The hormone prolactin is downregulated by dopamine and is upregulated by oestrogen. A falsely-high measurement may occur due to the presence of the biologically-inactive macroprolactin in the serum. This can show up as high prolactin in some types of tests, but is asymptomatic.
Treatment
Treatment is usually medication with dopamine agonists such as cabergoline,[8] bromocriptine (often preferred when pregnancy is possible),[9][10] and less frequently lisuride. A new drug in use is norprolac[11] with the active ingredient quinagolide. Terguride is also used.
Vitex agnus-castus extract can be tried in cases of mild hyperprolactinaemia.[12]
Historical names
The following eponyms were established before prolactin levels could be measured reliably in the clinical setting. On occasion, they are still encountered:
- Ahumada-DelCastillo syndrome, which refers to the association of galactorrhoea and amenorrhoea. It is also sometimes called Amenorrhoea-Galactorrhoea syndrome.[13]
- Chiari–Frommel syndrome, which refers to extended postpartum galactorrhoea and amenorrhoea.[14]
- Forbes–Albright syndrome, which refers to galactorrhoea-amenorrhoea associated with a pituitary tumour.[15]
References
- Mancini T, Casanueva FF, Giustina A (March 2008). "Hyperprolactinemia and prolactinomas". Endocrinology and Metabolism Clinics of North America. 37 (1): 67–99, viii. doi:10.1016/j.ecl.2007.10.013. PMID 18226731.
- Sabanegh ES (20 October 2010). Male Infertility: Problems and Solutions. Springer Science & Business Media. pp. 83–. ISBN 978-1-60761-193-6.
- Longo et al., Harrison's Principles of Internal Medicine, 18th ed., p.2887
- Torre DL, Falorni A (October 2007). "Pharmacological causes of hyperprolactinemia". Therapeutics and Clinical Risk Management. 3 (5): 929–51. PMC 2376090. PMID 18473017.
- Kantrowitz J, Citrome L (July 2008). "Paliperidone: the evidence of its therapeutic value in schizophrenia". Core Evidence. 2 (4): 261–71. PMC 3012441. PMID 21221191.
- Baumgartner A, Gräf KJ, Kürten I (July 1988). "Prolactin in patients with major depressive disorder and in healthy subjects. II. Longitudinal study of basal prolactin and post-TRH-stimulated prolactin levels". Biological Psychiatry. 24 (3): 268–85. doi:10.1016/0006-3223(88)90196-5. PMID 3135848.
- Peters F, Schuth W (March 1989). "Hyperprolactinemia and nonpuerperal mastitis (duct ectasia)". JAMA. 261 (11): 1618–20. doi:10.1001/jama.1989.03420110094030. PMID 2918655.
- Verhelst J, Abs R, Maiter D, van den Bruel A, Vandeweghe M, Velkeniers B, Mockel J, Lamberigts G, Petrossians P, Coremans P, Mahler C, Stevenaert A, Verlooy J, Raftopoulos C, Beckers A (July 1999). "Cabergoline in the treatment of hyperprolactinemia: a study in 455 patients". The Journal of Clinical Endocrinology and Metabolism. 84 (7): 2518–22. doi:10.1210/jc.84.7.2518. PMID 10404830.
- Webster J, Piscitelli G, Polli A, Ferrari CI, Ismail I, Scanlon MF (October 1994). "A comparison of cabergoline and bromocriptine in the treatment of hyperprolactinemic amenorrhea. Cabergoline Comparative Study Group". The New England Journal of Medicine. 331 (14): 904–9. doi:10.1056/NEJM199410063311403. PMID 7915824.
- Colao A, Di Sarno A, Guerra E, De Leo M, Mentone A, Lombardi G (April 2006). "Drug insight: Cabergoline and bromocriptine in the treatment of hyperprolactinemia in men and women". Nature Clinical Practice Endocrinology & Metabolism. 2 (4): 200–10. doi:10.1038/ncpendmet0160. PMID 16932285.
- Di Sarno A, Landi ML, Marzullo P, Di Somma C, Pivonello R, Cerbone G, Lombardi G, Colao A (July 2000). "The effect of quinagolide and cabergoline, two selective dopamine receptor type 2 agonists, in the treatment of prolactinomas". Clinical Endocrinology. 53 (1): 53–60. doi:10.1046/j.1365-2265.2000.01016.x. PMID 10931080.
- Kilicdag EB, Tarim E, Bagis T, Erkanli S, Aslan E, Ozsahin K, Kuscu E (June 2004). "Fructus agni casti and bromocriptine for treatment of hyperprolactinemia and mastalgia". International Journal of Gynaecology and Obstetrics. 85 (3): 292–3. doi:10.1016/j.ijgo.2004.01.001. PMID 15145274.
- Ahumada-del Castillo syndrome at Who Named It?
- Chiari-Frommel syndrome at Who Named It?
- Forbes-Albright syndrome at Who Named It?
External links
| Classification | |
|---|---|
| External resources |