Zeroing in on “nightmare bacteria” CRE hot spots in a Colorado hospital, 2012
The AMD program, which began in 2014, represents a significant leap forward for CDC’s advanced sequencing and bioinformatics capabilities. Prior to receiving AMD funding, CDC incorporated genetic sequencing methods in some infectious disease outbreak responses. This “AMD in Action” story about CDC’s pre-AMD funded work foreshadows the more robust and far-reaching effort launched in 2014—an escalated attack on infectious disease outbreaks that is proving to be better, quicker, and cheaper.
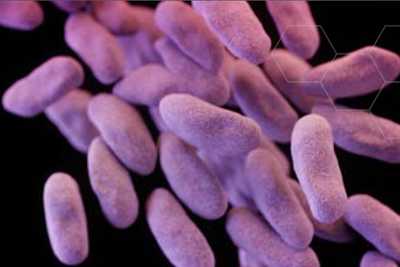
The diagnosis of a drug-resistant “nightmare bacteria” in two Colorado patients spurred hospital and state health officials to join forces with CDC to investigate. These bacteria — Carpabenem-resistant Enterobacteriaceae , or CRE — have become resistant to all or nearly all of the antibiotics we have today. Untreatable and hard-to-treat infections from CRE germs are on the rise among patients in medical facilities.
The Colorado outbreak was unique because it posed a new CRE threat. The bacteria contained an enzyme, NDM, not commonly seen in the United States.
In 2012, these cases marked the largest U.S. outbreak of the type of CRE caused by the enzyme NDM. Before this outbreak, only 16 isolates in clusters with two or fewer cases had been identified in the United States since 2009. And 14 of those were from patients who had received medical care overseas, where this type of CRE infection is common.
This outbreak concerned health officials because it demonstrated the risk for these organisms to spread inside American hospitals.
Standard testing methods showed the samples to be almost identical (90%–95% similar). But when CDC applied whole genome sequencing, scientists found the strains divided into three distinct clusters. By matching these clusters to patient movements and locations within the hospital, the scientists were able to track transmission of the bacteria to four specific places in the hospital.
Because whole genome sequencing provided additional information about where CRE was spreading in the hospital, investigators were able to zero in on these four hot spots to reinforce infection control measures and protect other patients from CRE. Whole genome sequencing can help pinpoint the links in outbreaks more quickly, and understanding these links can help investigators focus their efforts to interrupt spread of these “nightmare bacteria” as quickly as possible.
- Page last reviewed: August 17, 2015
- Page last updated: August 17, 2015
- Content source:
- Centers for Disease Control and Prevention
- Page maintained by: Office of Associate Director of Communication, Division of Public Affairs


 ShareCompartir
ShareCompartir