Fertility testing
Fertility testing is the process by which fertility is assessed, both generally and also to find the fertile window. General health affects fertility, and STI testing is an important related field.
| Fertility testing | |
|---|---|
| Medical diagnostics | |
 | |
| Purpose | assess fertility |
Women
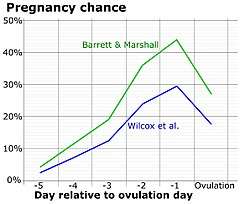
Healthy women are fertile from puberty until menopause, although fertility is typically much reduced towards the extremes of this period. The onset of puberty is typically identified by menarche and the presence of secondary sexual characteristics such as breast development, the appearance of pubic hair and changes to body fat distribution. The end of a woman's fertile years typically comes somewhat before menopause, as fertility declines to a point where establishing a viable pregnancy is very unlikely.
Ovulation testing
Various methods of predicting fertility exist, to either aid or avoid pregnancy.
Stretch test

Cervical mucus becomes clear and stretchy during the fertile window, to allow sperm to survive in and travel through it. The consistency of fertile mucous is akin to egg white.
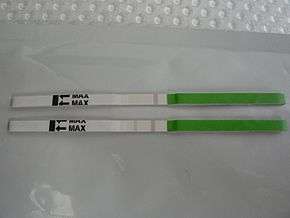
Ovulation prediction kit
Ovulation prediction kits are usually antibody tests for luteinising hormone, which peaks in urine around the time of ovulation. Some tests, such as the Clearblue fertility monitor, also test for estradiol.
Electronic fertility monitors
A fertility monitor is an electronic device which may use various methods to assist the user with fertility awareness. A fertility monitor may analyze changes in hormone levels in urine, basal body temperature, electrical resistance of saliva and vaginal fluids, or a combination of these methods. These devices may assist in pregnancy achievement. However, at the moment there is insufficient evidence available to draw conclusions on the effectiveness of fertility monitoring on live births or pregnancies.[2]
Cervical position
The cervix becomes soft, high, open and wet during the fertile window.
Basal Body Temperature Charting
Basal body temperature changes during the menstrual cycle. Higher levels of progesterone released during the menstrual cycle causes an abrupt increase in basal body temperature by 0.5 °C to 1 °C at the time of ovulation.[3] This enables identification of the fertile window through the use of commercial thermometers. This test can also indicate if there are issues with ovulation.[4]
Calendar methods
Because the fertile window arrives at approximately the same time each month, calendar methods can be used to predict ovulation.
Diagnosis of infertility
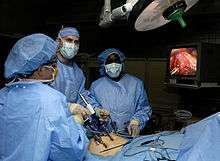
Women of fertile age may be infertile for a number of reasons. Various tests are available to establish reasons.
Anti-Müllerian hormone testing
Anti-Müllerian hormone tests allow the estimation of ovarian reserve. These give an indication of the likely remaining fertility opportunities a woman may have.
Follicle stimulating hormone
Tests for follicle stimulating hormone establish whether or not a woman will ovulate in any given month. This test is typically carried out on day 3 of the menstural cycle.
Hysterosalpingography
Hysterosalpingography involve the inspection of the fallopian tubes and uterus, by the injection of a radiocontrast agent, to ensure the egg can pass down the tube without obstruction, and to identify uterine abnormalities.
Ovarian ultrasound
Ultrasound scans of the ovaries may be conducted to establish the development of ovarian follicles. This can be useful particularly in the diagnosis of polycystic ovary syndrome.
Hysteroscopy
Hysteroscopy is used to diagnose the presence of a number of conditions which may affect fertility, such as uterine fibroids, Asherman's syndrome, and bicornate uterus. It involves the insertion of an endoscope to produce images of the inside of the uterus.
Laparoscopy
Laparoscopy is used to examine the interior of the abdomen. It can be used to establish patency of the fallopian tubes, and is especially suitable for the diagnosis of endometriosis.
Men
Males who have gone through puberty should be fertile throughout life. Men ejaculate semen which contains sex cells called sperm. After intercourse, sperm travel to the egg through the female reproductive tract, typically causing fertilisation to occur in the fallopian tubes.
Fertility testing for men involves semen testing and genetic testing, as other factors such as impotence are obvious. Semen can be tested for sperm count, sperm motility, sperm morphology, pH, volume, fructose content, and acrosome activity. Checks are also made to identify undescended testicles and retrograde ejaculation, along with medical history, such as cancer treatment, radiation, drug use, etc. In some cases the hamster zona-free ovum test may also be used to diagnose fertility. Genetic testing and chromosomal analysis can rule out some other causes of male infertility, such as Klinefelter syndrome.
A recent study identified epigenetic patterns in male sperm that may contribute to infertility.[5]
See also
References
- Dunson, D.B.; Baird, D.D.; Wilcox, A.J.; Weinberg, C.R. (1999). "Day-specific probabilities of clinical pregnancy based on two studies with imperfect measures of ovulation". Human Reproduction. 14 (7): 1835–1839. doi:10.1093/humrep/14.7.1835. ISSN 1460-2350.
- Manders, M; McLindon, L; Schulze, B; Beckmann, MM; Kremer, JA; Farquhar, C (17 March 2015). "Timed intercourse for couples trying to conceive". The Cochrane Database of Systematic Reviews. 3: CD011345. doi:10.1002/14651858.CD011345.pub2. PMID 25775926.
- Hall, John (2010). Guyton and Hall textbook of medical physiology (12th ed.). Philadelphia, Pa.: Saunders/Elsevier. ISBN 978-1416045748.
- "Infertility Diagnosis". ARC Fertility. Retrieved 4 November 2016.
- Kenneth I. Aston; Philip J. Uren; Timothy G. Jenkins; Alan Horsager; Bradley R. Cairns; Andrew D. Smith; Douglas T. Carrell (December 2015). "Aberrant sperm DNA methylation predicts male fertility status and embryo quality". Fertility and Sterility. 104 (6): 1388–1397. doi:10.1016/j.fertnstert.2015.08.019. PMID 26361204.