Blood Lead Levels in Children Aged <5 Years — United States, 2007–2013
Weekly / October 14, 2016 / 63(55);66–72
Preface
This report provides data concerning childhood blood lead levels (BLLs) in the United States during 2007–2013. These data were collected and compiled from raw data extracts sent by state and local health departments to CDC’s Childhood Blood Lead Surveillance (CBLS) system. These raw data extracts have been de-identified and coded into a format specifically for childhood lead reporting. The numbers of children aged <5 years reported to CDC for 2013 with newly confirmed BLLs ≥10 µg/dL are provided in tabular form by month (Table 1) and geographic location (Table 2). The incidence of BLLs ≥10 µg/dL is reported by age group for 2007–2013 (Table 3). The numbers of children aged <5 years with BLLs 5–9µg/dL for 2013 are reported (Table 4). For the period 2007–2013, the numbers of children newly confirmed with BLLs ≥70 µg/dL are summarized (Figure 1) as well as the percentage of children with BLLs ≥5 µg/dL (Figure 2). This report is a part of the Summary of Notifiable Noninfectious Conditions and Disease Outbreaks — United States, which encompasses various surveillance years but is being published in 2016 (1). The Summary of Notifiable Noninfectious Conditions and Disease Outbreaks appears in the same volume of MMWR as the annual Summary of Notifiable Infectious Diseases (2).
Background
Permanent neurologic damage and behavioral disorders have been found to be associated with lead exposure at blood levels at or below 5 µg/dL (3–6). No safe BLLs in children have been identified (7). Studies examining children with high BLLs (≥70 µg/dL) have shown severe neurologic problems, including seizures, comas, and death (8). Children aged <5 years are at increased risk because their bodies are growing rapidly and they tend to put their hands or other objects, which might be contaminated with lead dust, into their mouths.
In 1991, CDC recommended that BLLs ≥10 µg/dL in children should prompt public health action by the state or local health departments with follow-up testing (9). In 1995, the Council of State and Territorial Epidemiologists (CSTE), in collaboration with CDC, designated elevated BLLs as the first noninfectious condition to be added to the list of conditions designated as reportable at the national level (10).
In May 2012, the Advisory Committee on Childhood Lead Poisoning Prevention* (ACCLPP) recommended the use of a reference range for blood lead (11). ACCLPP recommended that the upper value of the reference range be based on the 97.5th percentile of the National Health and Nutritional Examination Survey† (NHANES). A generated BLL distribution in children aged 1–5 years (currently 5 µg/dL) is used by clinical and public health care providers to identify children with elevated BLLs (11).
In 2012, a total of 29 states and New York City identified and reported approximately 138,000 children aged <6 years with BLLs ≥5 µg/dL (12). Federal funding for reporting BLLs ended in 2012, and several states lost their statewide lead programs. By 2013, the number of children reported to CDC with BLLs ≥5 µg/dL had decreased, as had the number of states reporting data to CDC (12). For this report, CDC examined reported BLLs of children aged <5 years in three categories: children with BLLs ≥10 µg/dL, children with new reports of BLLs ≥10 µg/dL, and children with BLLs 5–9µg/dL.)
Data Sources
Results of blood lead tests for children from state and local health departments were sent to CDC’s Healthy Homes and Lead Poisoning Prevention Program (HHLPPP). When federal funding was available, prior to 2013, states submitted data on a quarterly basis. After funding ended in 2012, a total of 27 states, the District of Columbia, and New York City continued to submit data to CDC in 2013 while 14 states that had lost funding for their childhood lead program could not provide data. Most of the states that continued to have childhood lead programs had sustainable funding through the state in which the health departments would verify the data collected for blood lead testing. The test results compiled and analyzed by state health departments and submitted to CDC comprise the CBLS database.
State and local childhood blood lead surveillance systems retain the results of blood lead tests of children reported to state health departments by private laboratories, as well as state and local government laboratories. The reporting criteria of BLLs from the laboratories to the state are set by each state and vary across jurisdictions. A set of core data variables have been established by CDC and participating states that should be collected for every child at the time of the blood lead test. These variables include identification and demographic information (e.g., date of birth, race, or ethnicity), laboratory information (e.g., venous or capillary blood test), date of blood lead test, address information such as city and zip code, and test result (13). Each child is assigned a unique identifier that corresponds to the de-identified and de-duplicated data sent to CDC. CDC checks each state-submitted record for correct formatting, coding and content. Records not meeting CDC criteria are summarized in file processing reports that are sent to states for correction. Certain errors, if not corrected, prevent the record from being entered in CDC’s CBLS database. For states with an error rate >10%, no data are loaded into CBLS, and the state must correct the problems before sending the records back to CDC.
Interpreting Data
In this report, state surveillance data are presented for children aged <5 years who were tested for lead at least once during 2007–2013 and whose tests were reported to CDC. Having a confirmed BLL ≥10 µg/dL is defined as having one venous blood lead test ≥10 µg/dL or two capillary blood lead tests ≥10 µg/dL drawn within 12 weeks of each other (14). Incidence data rates are presented by the date of the confirmed blood lead test. Data are reported by the jurisdiction of the child’s residence at the time of the confirmed blood lead test. State health departments check for duplicate laboratory reports for children and completeness of the laboratory report before sending the data to CDC. After data are sent, CDC also checks to ensure the completeness and accuracy of the data.
The data provided in this report are useful for analyzing childhood blood lead trends and determining relative morbidity numbers. However, reporting practices affect how these data are interpreted. Childhood blood lead reporting is likely incomplete, and completeness of the records might vary depending on state, laboratory, or BLL range (e.g., BLLs <10 µg/dL might not be required to be reported in some states). Independent of the actual incidence of disease, factors such as changes in the methods of surveillance or introduction of new diagnostic tests (e.g., use of a portable handheld analyzer) can cause changes in the reported blood lead levels.
In 2007, a total of 38 states, New York City, and the District of Columbia reported data to CDC. During 2007–2013, the number of states collecting and reporting childhood blood lead data to CDC fluctuated. Federal funding from CDC to state and local health departments ended in September 2012. For this reason, no states were required to report childhood blood lead data to CDC in 2013. Nevertheless, 29 jurisdictions (27 states, New York City, and the District of Columbia) did collect and report data to CDC. Although the varying number of states reporting data from year to year during 2007–2013 limits the extent to which trends can be analyzed, the data nonetheless can indicate BLLs in children for a particular year.
Methods for Identifying Childhood Blood Lead
Elevated blood lead levels has been a notifiable condition since 1995 (9). CDC asks state health departments to report all blood lead test data for children to HHLPPP, regardless of the BLL. Each state has its own laws and regulations regarding blood lead test reporting to the state health department. Of the 35 programs funded in 2014 by CDC, 33 required electronic reporting from the laboratory to the state health department.
Before ACCLPP’s mid-2012 recommendation to use the 97.5 percentile from NHANES, currently 5 µg/dL, the “level of concern” was 10 µg/dL (10). For this report, elevated BLLs are defined as confirmed BLLs ≥10 µg/dL. Data on children with BLLs ≥5 µg/dL also are reported.
Highlights
Lead exposure in children can cause permanent neurologic damage (3). Behavioral disorders are associated with lead exposure even at detectable blood levels at or below 5 µg/dL (3–6). The most common highly concentrated source of lead for children in the United States is lead paint. When paint containing lead deteriorates into flakes, chips, or fine dust, it is easily inhaled or ingested by small children.
In 2011, the last full calendar year of federal funding from CDC, 34 states§, District of Columbia, and New York City submitted BLL data to CDC; however, by 2013, only 27 states¶, District of Columbia, and New York City submitted data (a 21% reduction in contributors). Although the decline in the number of health departments submitting data to CDC makes it difficult to assess trends over time, it is still possible to evaluate new cases in children with confirmed BLLs ≥10 µg/dL and cases in children with BLL 5–9 µg/dL from the states that continue to submit data to CDC.
In 2013, during the warmest weather months (July–September), 2,965 new cases were identified, more than in any other consecutive 3-month period (Table 1). In warm weather, windows that possibly are painted with lead-based paint are opened and closed, creating lead dust in the air and on the ground. Repainting and renovation activities also are more common in warm-weather months. Increased presence and activity of children in and around the home might lead to children having more contact with contaminated dust, surfaces, and soil (15). This contact can lead to higher BLLs in the late summer and early fall.
The East North Central region reported the greatest number of new cases in 2013, with 2,997 children aged <5 years with confirmed BLLs ≥10 µg/dL reported to CDC, followed by the Mid-Atlantic region with 2,472 children (Table 2). These two regions (comprising eight state and local health departments that reported data) accounted for 67% of the new cases in the United States and almost 47% of the children aged <5 years tested and reported to CDC for 2013. The other seven geographic areas (comprising 21 state and local health departments that reported data to CDC for 2013) accounted for the remaining 33% of new cases and for 53% of the children aged <5 years tested and reported to CDC for 2013.
The number of new cases, defined as cases in children aged <5 years with a first-ever confirmed BLL ≥10 µg/dL, that were reported to CDC continued to decrease during 2007–2013 (Table 3). Although not all jurisdictions reported data to CDC, the denominator is the entire child population aged <1 year and aged 1–4 years from the U.S. Census across all years. Children aged 1–4 years continue to have a higher rate of confirmed BLLs ≥10 µg/dL than other children across all years, possibly because of increased hand-to-mouth activity and mobility for older children.
The numbers of newly confirmed children with BLLs ≥70 µg/dL during 2007–2013 are presented in graphic form (Figure 1). Changes in the number of jurisdictions reporting data to CDC over these 7 years make it difficult to discern any trend or clear pattern. One Healthy People 2010 environmental health objective is eliminating BLLs ≥10 µg/dL (16). These children have BLLs at least seven times above the Healthy People 2010 goal.
Prealence data indicate that 74,110 children aged <5 years had a BLL 5–9µg/dL in 2013 (Table 4). Although a single capillary test is not a confirmatory test, in 2013, of the approximately 74,000 children aged <5 years who were tested and who were reported to CDC as having BLLs 5–9µg/dL, 31,779 ( 43%) had a confirmed 5–9 µg/dL by venous sample type. The mid-2012 change in the reference value and the loss of federal funding to state and local health departments from CDC made it difficult for most states to extend follow up testing for capillary tests 5–9µg/dL. Although venous blood lead samples have been the gold standard, one study has shown that capillary blood draws are suitable alternatives to venous blood draws when screening children aged <6 years to determine lead exposure and provide reasonable estimates at the population level (17).
During 2007–2013, a majority of the children aged <5 years with BLLs ≥5 µg/dL had BLLs 5–9 µg/dL (Figure 2). The percentage of children with confirmed BLLs ≥10 µg/dL increased from 7.5% to 13.3% during the same period. CDC, along with state and local health departments, continue efforts to reduce BLLs ≥5 µg/dL and confirmed BLLs ≥10 µg/dL through screening and primary prevention (18).
Effective surveillance requires state and local health departments to track a substantial number of children and their blood lead test results over time. More detailed annual summaries describing the number of children tested for lead by state, county, and BLL are published periodically by CDC. A summary of childhood lead exposure in 2014, the most recent year for which data are available, is provided at http://www.cdc.gov/nceh/lead.
Corresponding author: Jaime Raymond, Division of Emergency and Environmental Health Services, National Center for Environmental Health, CDC. Telephone: 770-488-3627; E-mail: zvu0@cdc.gov.
1Division of Emergency and Environmental Health Services, National Center for Environmental Health, CDC
References
- CDC. Summary of notifiable noninfectious conditions and disease outbreaks—United States. MMWR Morb Mortal Wkly Rep 2013;63(55).
- CDC. Summary of notifiable infectious diseases and conditions—United States, 2014. MMWR Morb Mortal Wkly Rep 2014;63(54).
- Bellinger DC, Needleman HL. Intellectual impairment and blood lead levels. N Engl J Med 2003;349:500–2. CrossRef PubMed
- Bellinger DC, Stiles KM, Needleman HL. Low-level lead exposure, intelligence and academic achievement: a long-term follow-up study. Pediatrics 1992;90:855–61. PubMed
- Dietrich KN, Succop PA, Berger OG, Bornschein RL. Early exposure to lead and juvenile delinquency. Neurotoxicol Teratol 2001;23:511–8. CrossRef PubMed
- Needleman HL, McFarland C, Ness RB, Fienberg SE, Tobin MJ. Bone lead levels in adjudicated delinquents. A case control study. Neurotoxicol Teratol 2002;24:711–7. CrossRef PubMed
- CDC. Healthy homes and lead poisoning prevention: what do parents need to know to protect their children? Atlanta, GA: US Department of Health and Human Services, CDC; 2012. http://www.cdc.gov/nceh/lead/acclpp/blood_lead_levels.htm
- National Research Council. Measuring lead exposure in infants, children, and other sensitive populations. Washington, DC: National Academy Press; 1993.
- CDC. Preventing lead poisoning in young children: a statement by the Centers for Disease Control. Atlanta, GA: US Department of Health and Human Services, CDC; 1991. http://wonder.cdc.gov/wonder/prevguid/p0000029/p0000029.asp
- CDC. Changes in national notifiable diseases data presentation. MMWR Morb Mortal Wkly Rep 1996;45:41–2.
- CDC. Low level lead exposure harms children: a renewed call for primary prevention: report of the Advisory Committee on Childhood Lead Poisoning Prevention of the Centers for Disease Control and Prevention. Atlanta, GA: US Department of Health and Human Services, CDC; 2012. http://www.cdc.gov/nceh/lead/ACCLPP/Final_Document_030712.pdf
- CDC. Healthy Homes and Lead Poisoning Prevention: CDC’s national surveillance data (1997–2014). Atlanta, GA: US Department of Health and Human Services, CDC; 2012. http://www.cdc.gov/nceh/lead/data/Website_StateConfirmedByYear_1997_2014_01112016.htm
- CDC. Healthy Homes and Lead Poisoning Prevention: standard surveillance definitions and classifications. Atlanta, GA: US Department of Health and Human Services, CDC; 2016. http://www.cdc.gov/nceh/lead/data/definitions.htm
- Council of State and Territorial Epidemiologists. CSTE position statement 09-OH-02. Atlanta, GA: Council of State and Territorial Epidemiologists; 2009. http://c.ymcdn.com/sites/www.cste.org/resource/resmgr/PS/09-OH-02.pdf
- CDC. Children with elevated blood lead levels attributed to home renovation and remodeling activities—New York, 1993–1994. MMWR Morb Mortal Wkly Rep 1997;45:1120–3. PubMed
- US Department of Health and Human Services. Healthy people 2010: understanding and improving health. 2nd ed. 2 vols. Rockville, MD: US Government Printing Office; 2000. http://www.healthypeople.gov/2010
- Schlenker TL, Fritz CJ, Mark D, et al. Screening for pediatric lead poisoning: comparability of simultaneously drawn capillary and venous blood samples. JAMA 1994;271:1346–8. CrossRef PubMed
- Meyer PA, Pivetz T, Dignam TA, Homa DM, Schoonover J, Brody D. Surveillance for elevated blood lead levels among children—United States, 1997–2001. MMWR Surveill Summ 2003;52(No. SS-10):1–21. PubMed
* ACCLPP advised and guided the Secretary and Assistant Secretary of the U.S. Department of Health and Human Services and the Director of CDC regarding new scientific knowledge and technical developments and their practical implications for childhood lead poisoning prevention efforts (http://www.cdc.gov/nceh/lead/acclpp/acclpp_main.htm).
† NHANES is a program of studies designed to assess the health and nutritional status of adults and children in the United States (http://www.cdc.gov/nchs/nhanes.htm).
§ States and jurisdictions reporting data included Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, New Hampshire, New Jersey, New York, New York City, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Texas, Vermont, Virginia, Washington, West Virginia, and Wisconsin.
¶ States and jurisdictions reporting data included Alabama, Arizona, District of Columbia, Georgia, Illinois, Indiana, Kentucky, Maryland, Massachusetts, Minnesota, Mississippi, Missouri, New Hampshire, New Jersey, New York City, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Vermont, West Virginia, and Wisconsin.
 TABLE 1. Number and percentage of reported new cases of blood lead levels ≥10 µg/dL among children aged <5 years, by month — Childhood Blood Lead Surveillance System, United States, 2013*
TABLE 1. Number and percentage of reported new cases of blood lead levels ≥10 µg/dL among children aged <5 years, by month — Childhood Blood Lead Surveillance System, United States, 2013*
| Jan | Feb | Mar | Apr | May | June | July | Aug | Sept | Oct | Nov | Dec | Total No. |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| No. (%) | No. (%) | No. (%) | No. (%) | No. (%) | No. (%) | No. (%) | No. (%) | No. (%) | No. (%) | No. (%) | No. (%) | |
| 538 (6.5) | 469 (5.7) | 416 (5.1) | 543 (6.6) | 718 (8.7) | 739 (9.0) | 947 (11.5) | 1,053 (12.8) | 965 (11.7) | 823 (10.0) | 566 (6.0) | 453 (5.5) | 8,230 |
*A total of 29 jurisdictions reported data to CDC (Alabama, Arizona, Connecticut, District of Columbia, Georgia, Illinois, Indiana, Kentucky, Louisiana, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, New Jersey, New Hampshire, New Mexico, New York City, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Tennessee, Vermont, West Virginia, and Wisconsin).
 TABLE 2. Reported number of newly identified cases of blood lead levels ≥10 µg/dL among children aged <5 years, by geographic region and state — Childhood Blood Lead Surveillance System, United States, 2013
TABLE 2. Reported number of newly identified cases of blood lead levels ≥10 µg/dL among children aged <5 years, by geographic region and state — Childhood Blood Lead Surveillance System, United States, 2013
| Region/State | No. |
|---|---|
| 8,230 | |
| New England | 1,003 |
| Connecticut | 264 |
| Maine | —* |
| Massachusetts | 472 |
| New Hampshire | 75 |
| Rhode Island | 163 |
| Vermont | 29 |
| Mid-Atlantic | 2,472 |
| New Jersey | 593 |
| New York | — |
| New York City | 639 |
| Pennsylvania | 1,240 |
| Eastern North Central | 2,997 |
| Illinois | 1094 |
| Indiana | 183 |
| Michigan | 335 |
| Ohio | 941 |
| Wisconsin | 444 |
| Western North Central | 604 |
| Iowa | — |
| Kansas | — |
| Minnesota | 126 |
| Missouri | 478 |
| Nebraska | — |
| North Dakota | — |
| South Dakota | — |
| South Atlantic | 553 |
| Delaware | — |
| District of Columbia | 27 |
| Florida | — |
| Georgia | 136 |
| Maryland | 268 |
| North Carolina | 95 |
| South Carolina | — |
| Virginia | — |
| West Virginia | 27 |
| Eastern South Central | 269 |
| Alabama | 72 |
| Kentucky | 49 |
| Mississippi | 71 |
| Tennessee | 77 |
| Western South Central | 241 |
| Arkansas | — |
| Louisiana | 120 |
| Oklahoma | 121 |
| Texas | — |
| Mountain | 83 |
| Arizona | 69 |
| Colorado | — |
| Idaho | — |
| Montana | — |
| Nevada | — |
| New Mexico | 14 |
| Utah | — |
| Wyoming | — |
| Pacific | 8 |
| Alaska | — |
| California | — |
| Hawaii | — |
| Oregon | 8 |
| Washington | — |
* No data were reported for 2013.
 TABLE 3. Reported number of new cases and incidence rate per 100,000 children aged <5 years with blood lead levels ≥10 µg/dL, by age group — Childhood Blood Lead Surveillance System, United States, 2007–2013*
TABLE 3. Reported number of new cases and incidence rate per 100,000 children aged <5 years with blood lead levels ≥10 µg/dL, by age group — Childhood Blood Lead Surveillance System, United States, 2007–2013*
| Year | <1 yr | 1–4 yrs | ||
|---|---|---|---|---|
| No. | Rate | No. | Rate | |
| 2007† | 2,055 | 47.75 | 18,398 | 110.72 |
| 2008§ | 1,852 | 43.00 | 15,251 | 90.41 |
| 2009¶ | 1,608 | 38.69 | 13,432 | 78.76 |
| 2010** | 1,412 | 34.05 | 11,647 | 68.05 |
| 2011†† | 1,185 | 29.89 | 10,532 | 65.25 |
| 2012§§ | 860 | 21.81 | 9,369 | 58.31 |
| 2013¶¶ | 777 | 19.55 | 7,453 | 46.89 |
*Denominators are calculated as estimates of all children living in the United States from U.S. Census data.
†A total of 40 jurisdictions reported data to CDC (Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, Nebraska, Nevada, New Jersey, New Hampshire, New York, New York City, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Tennessee, Texas, Vermont, Virginia, Washington, West Virginia, and Wisconsin).
§A total of 38 jurisdictions reported data to CDC (Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, Nevada, New Jersey, New Hampshire, New York, New York City, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Texas, Vermont, Virginia, Washington, West Virginia, and Wisconsin).
¶A total of 38 jurisdictions reported data to CDC (Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, Nevada, New Jersey, New Hampshire, New York, New York City, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Texas, Vermont, Virginia, Washington, West Virginia, and Wisconsin).
**A total of 37 jurisdictions reported data to CDC (Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, Nevada, New Jersey, New Hampshire, New York, New York City, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Texas, Vermont, Virginia, Washington, West Virginia, and Wisconsin).
††A total of 36 jurisdictions reported data to CDC (Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, New Jersey, New Hampshire, New York, New York City, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Texas, Vermont, Virginia, Washington, West Virginia, and Wisconsin).
§§A total of 30 jurisdictions reported data to CDC (Alabama, Arizona, Connecticut, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, New Jersey, New Hampshire, New York, New York City, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Vermont, West Virginia, and Wisconsin).
¶¶A total of 29 jurisdictions reported data to CDC (Alabama, Arizona, Connecticut, District of Columbia, Georgia, Illinois, Indiana, Kentucky, Louisiana, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, New Jersey, New Hampshire, New Mexico, New York City, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Tennessee, Vermont, West Virginia, and Wisconsin).
 TABLE 4. Number of children aged <5 years with blood lead levels 5–9 µg/dL, by sample type and age — Childhood Blood Lead Surveillance System, United States, 2013*
TABLE 4. Number of children aged <5 years with blood lead levels 5–9 µg/dL, by sample type and age — Childhood Blood Lead Surveillance System, United States, 2013*
| Age at time of blood lead test (yrs) | Capillary/Unknown (%) | Venous (%) |
|---|---|---|
| <1 | 3,960 (61.2) | 2,510 (38.8) |
| 1 | 14,035 (56.4) | 10,866 (43.6) |
| 2 | 11,999(57.2) | 8,967 (42.8) |
| 3 | 6,728 (57.2) | 5,028 (42.8) |
| 4 | 5,609 (56.0) | 4,408 (44.0) |
| Total | 42,331 (57.1) | 31,779 (42.9) |
*A total of 29 jurisdictions reported data to CDC (Alabama, Arizona, Connecticut, District of Columbia, Georgia, Illinois, Indiana, Kentucky, Louisiana, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, New Jersey, New Hampshire, New Mexico, New York City, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Tennessee, Vermont, West Virginia, and Wisconsin).
 FIGURE 1. Number of children aged <5 years with newly confirmed blood lead levels =70µgL — Childhood Blood Lead Surveillance System, United States, 2007–2013*
FIGURE 1. Number of children aged <5 years with newly confirmed blood lead levels =70µgL — Childhood Blood Lead Surveillance System, United States, 2007–2013*
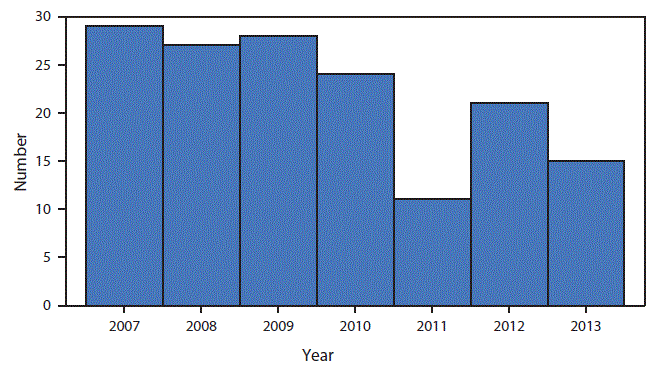
*For 2007, a total of 40 jurisdictions reported data to CDC (Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, Nebraska, Nevada, New Jersey, New Hampshire, New York, New York City, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Tennessee, Texas, Vermont, Virginia, West Virginia, and Wisconsin).
For 2008, a total of 39 jurisdictions reported data to CDC (Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Nebraska, Nevada, New Jersey, New Hampshire, New York, New York City, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Tennessee, Texas, Vermont, Virginia, West Virginia, and Wisconsin).
For 2009, a total of 39 jurisdictions reported data to CDC (Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, Nevada, New Jersey, New Hampshire, New York, New York City, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Tennessee, Texas, Vermont, Virginia, West Virginia, and Wisconsin).
For 2010, a total of 37 jurisdictions reported data to CDC (Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, Nevada, New Jersey, New Hampshire, New York, New York City, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Texas, Vermont, Virginia, West Virginia, and Wisconsin).
For 2011, a total of 36 jurisdictions reported data to CDC (Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, New Jersey, New Hampshire, New York, New York City, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Texas, Vermont, Virginia, Washington, West Virginia, and Wisconsin).
For 2012, a total of 30 jurisdictions reported data to CDC (Alabama, Arizona, Connecticut, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, New Jersey, New Hampshire, New York, New York City, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Vermont, West Virginia, and Wisconsin).
For 2013, a total of 29 jurisdictions reported data to CDC (Alabama, Arizona, Connecticut, District of Columbia, Georgia, Illinois, Indiana, Kentucky, Louisiana, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, New Jersey, New Hampshire, New Mexico, New York City, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Tennessee, Vermont, West Virginia, and Wisconsin).
 FIGURE 2. Percentage of children aged <5 years with BLLs =5 µg/dL, by year and blood lead level — Childhood Blood Lead Surveillance System, United States, 2007–2013*United States, 2007–2013*
FIGURE 2. Percentage of children aged <5 years with BLLs =5 µg/dL, by year and blood lead level — Childhood Blood Lead Surveillance System, United States, 2007–2013*United States, 2007–2013*
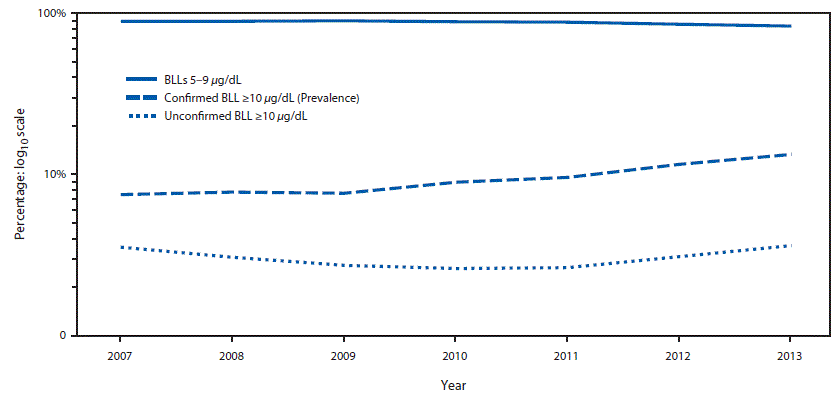
*For 2007, a total of 40 jurisdictions reported data to CDC (Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, Nebraska, Nevada, New Jersey, New Hampshire, New York, New York City, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Tennessee, Texas, Vermont, Virginia, West Virginia, and Wisconsin).
For 2008, a total of 39 jurisdictions reported data to CDC (Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Nebraska, Nevada, New Jersey, New Hampshire, New York, New York City, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Tennessee, Texas, Vermont, Virginia, West Virginia, and Wisconsin).
For 2009, a total of 39 jurisdictions reported data to CDC (Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, Nevada, New Jersey, New Hampshire, New York, New York City, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Tennessee, Texas, Vermont, Virginia, West Virginia, and Wisconsin).
For 2010, a total of 37 jurisdictions reported data to CDC (Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, Nevada, New Jersey, New Hampshire, New York, New York City, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Texas, Vermont, Virginia, West Virginia, and Wisconsin).
For 2011, a total of 36 jurisdictions reported data to CDC (Alabama, Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, New Jersey, New Hampshire, New York, New York City, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Texas, Vermont, Virginia, Washington, West Virginia, and Wisconsin).
For 2012, a total of 30 jurisdictions reported data to CDC (Alabama, Arizona, Connecticut, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, New Jersey, New Hampshire, New York, New York City, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Vermont, West Virginia, and Wisconsin).
For 2013, a total of 29 jurisdictions reported data to CDC (Alabama, Arizona, Connecticut, District of Columbia, Georgia, Illinois, Indiana, Kentucky, Louisiana, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, New Jersey, New Hampshire, New Mexico, New York City, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Tennessee, Vermont, West Virginia, and Wisconsin).
Suggested citation for this article: Raymond J, Brown MJ. Blood Lead Levels in Children Aged <5 Years — United States, 2007–2013. MMWR Morb Mortal Wkly Rep 2016;63:66–72. DOI: http://dx.doi.org/10.15585/mmwr.mm6355a6.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All HTML versions of MMWR articles are generated from final proofs through an automated process. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (https://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.
- Page last reviewed: July 19, 2017
- Page last updated: July 19, 2017
- Content source:


 ShareCompartir
ShareCompartir