Campylobacter
Campylobacter (meaning "curved bacteria") is a genus of Gram-negative bacteria.[1] Campylobacter typically appear comma- or s-shaped, and are motile.[1]
| Campylobacter | |
|---|---|
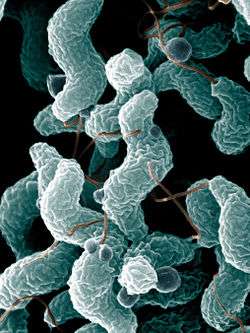 | |
| Campylobacter jejuni | |
| Scientific classification | |
| Domain: | Bacteria |
| Phylum: | |
| Class: | |
| Order: | |
| Family: | |
| Genus: | Campylobacter Sebald & Véron, 1963 |
| Species | |
|
C. avium | |
Most Campylobacter species can infect humans and other animals, causing disease. The bacterium's main natural reservoir is poultry;[2] humans can contract the disease from eating food contaminated with Campylobacter species. Another source of infection is contact with infected animals, which often carry Campylobacter asymptomatically.[3] At least a dozen species of Campylobacter have been implicated in human disease, with C. jejuni and C. coli being the most common.[4] C. jejuni is now recognized as one of the main causes of bacterial foodborne disease in many developed countries.[4][5] C. jejuni infection can also spread to the blood in individuals with AIDS, while C. lari is a known cause of recurrent diarrhea in children.[3] C. fetus is a cause of spontaneous abortions in cattle and sheep, as well as an opportunistic pathogen in humans.[6] This genus has been found to be part of the salivary microbiome.[7]
Description
Campylobacter species generally appear as curved or comma-shaped rods, and are able to move via unipolar or bipolar flagella.[1] They generally survive in environments with low oxygen. When exposed to atmospheric oxygen, C. jejuni is able to change into a coccal form [8] They are positive by the oxidase test and catalase test. Campylobacter spp. are nonfermentative,[1] and are best cultured at 42 °C.[8]
Survival at room temperature is poor, but they can survive for a short time at refrigeration temperatures – up to 15 times longer at 2 °C than at 20 °C. The bacterium dies out slowly at freezing temperatures and is heat sensitive: the cells are destroyed at temperatures above 48 °C.[9]
History
The symptoms of Campylobacter infection were described in 1886 in infants by Theodor Escherich.[10] These infections were named cholera infantum,[10] or summer complaint.[11] The species was first isolated by Sir John McFadyean, of the Royal Veterinary College in London, in 1906.[12]
The genus was further defined in 1963.[13]
Genetics
The genomes of several Campylobacter species have been sequenced, beginning with C. jejuni in 2000.[14][15] These genome studies have identified molecular markers specific to members of Campylobacter. Additionally, several markers were found in all Campylobacter species except for C. fetus, the most distantly related species. Many markers were also found which were conserved only between C. jejuni and C. coli, indicating a close relationship between these two species.[16]
Similar studies have investigated the genes responsible for motility in Campylobacter species. All Campylobacter species contain two flagellin genes in tandem for motility, flaA and flaB. These genes undergo intergenic recombination, further contributing to their virulence.[17]
The number of known quinolone-resistant strains is growing. Evidence suggests this is caused by an overuse of this class of antibiotics in animal agriculture.[8]
Bacteriophage
The confusing taxonomy of Campylobacter over the past decades makes identifying the earliest reports of Campylobacter bacteriophages difficult. Bacteriophages specific to the species now known as C. coli and C. fetus (previously Vibrio coli and V. fetus), were first isolated from cattle and pigs during the 1960s, and Campylobacter bacteriophage therapy is an ongoing area of research in the age of bacterial antibiotic resistance.[18][19][20][21]
Pathogenesis
Campylobacter can cause a gastrointestinal infection called campylobacteriosis. The incubation period is 24–72 hours after infection.[22] This is characterized by an inflammatory, sometimes bloody diarrhea or dysentery syndrome, mostly including cramps, fever, and pain.[23][24] The most common routes of transmission are fecal-oral, ingestion of contaminated food or water, and the eating of raw meat. Foods implicated in campylobacteriosis include raw or under-cooked poultry, raw dairy products, and contaminated produce.[25] Campylobacter is sensitive to the stomach's normal production of hydrochloric acid: as a result, the infectious dose is relatively high, and the bacteria rarely cause illness when a person is exposed to less than 10,000 organisms.[3] Nevertheless, people taking antacid medication (e. g. people with gastritis or stomach ulcers) are at higher risk of contracting disease from a smaller number of organisms, since this type of medication neutralizes normal gastric acid.
In humans, the sites of tissue injury include the jejunum, the ileum, and the colon. Most strains of C jejuni produce cytolethal distending toxin, which inhibits cell division and impedes activation of the immune system. This helps the bacteria to evade the immune system and survive for a limited time inside intestinal cells. A cholera-like enterotoxin was also, at one time, believed to be produced, but this appears not to be the case. The organism produces diffuse, bloody, edematous, and exudative enteritis. Campylobacter has, on rare occasions, been blamed for hemolytic uremic syndrome and thrombotic thrombocytopenic purpura, though no unequivocal case reports exist. In some cases, a Campylobacter infection can be the underlying cause of Guillain–Barré syndrome. Gastrointestinal perforation is a rare complication of ileal infection.[26]
Campylobacter has also been associated with periodontitis.[23]
Treatment
The infection is usually self-limiting and, in most cases, symptomatic treatment by liquid and electrolyte replacement is sufficient to treat human infections. Symptoms typically last 5–7 days.[25] Treatment with antibiotics has little effect, and is discouraged except in high-risk patients.[27] Diagnosis of campylobacteriosis is made by testing a fecal specimen. Standard treatment in high-risk cases is azithromycin, a macrolide antibiotic, especially for Campylobacter infections in children,[28] although other antibiotics, such as quinolones, tetracycline and other macrolides are sometimes used to treat gastrointestinal Campylobacter infections in adults.[29] In case of systemic infection, other bactericidal antibiotics are used, such as ampicillin, amoxicillin/clavulanic acid, or aminoglycosides. Fluoroquinolone antibiotics, such as ciprofloxacin or levofloxacin, may no longer be effective in some cases, due to resistance.[30] In addition to antibiotics, dehydrated children may require intravenous fluid treatment in a hospital.
Epidemiology
UK
In January 2013, the UK's Food Standards Agency (FSA) warned that two-thirds of all raw chicken bought from UK shops was contaminated with Campylobacter, affecting an estimated half a million people annually and killing about 100 of them.[31] In June 2014, the FSA started a campaign against washing raw chicken, as washing can spread germs onto clean surfaces by splashing.[32] In May 2015, cumulative results for samples taken from fresh chickens between February 2014 and February 2015 were published by the FSA and showed 73% of chickens tested positive for the presence of Campylobacter.[33]
USA
Campylobacter infections increased 14% in the United States in 2012 compared to the rate from 2006 to 2008. This represents the highest reported number of infections since calendar year 2000.[25]
High prevalence of Campylobacter (40% or more) has been reported in raw chicken meat in regional retail stores in the USA, which remained steady from 2005 through 2011.[34] The last USDA quarterly progress report on Salmonella and Campylobacter testing of meat and poultry, for July–September 2014, showed a low prevalence of Campylobacter spp. in ground chicken meat, but a larger prevalence (20%) in mechanically separated chicken meat (which is sold only for further processing).[35]
Canada
FoodNet Canada has reported that Campylobacter was the most common pathogen found on packaged chicken breast, with nearly half of all samples testing positive. Additionally, Campylobacter and Salmonella were the most common causes of gastrointestinal illness in Canada.[36]
New Zealand
In August 2016, an estimated 4,000+ residents of Havelock North, a town with around 13,000 residents, had gastric illness after the water supply was thought to be contaminated by Campylobacter.[37][38]
Norway
In June 2019, an estimated 2,000 residents of Askøy municipality got sick due to the presence of Campylobacter in the water supply.[39]
References
- Vandamme, Peter; Dewhirst, Floyd E.; Paster, Bruce J.; On, Stephen L.W. (2006). Garrity, George; Brenner, Don J.; Staley, James T.; Krieg, Noel R.; Boone, David R.; DeVos, Paul; Goodfellow, Michael; Rainey, Fred A.; Schleifer, Karl-Heinz (eds.). Bergey's Manual of Systematic Bacteriology: Volume Two: The Proteobacteria (Part C) (2nd ed.). Springer Science & Business Media. pp. 1147–1160. ISBN 978-0-387-29298-4.
- "Infectious disease Campylobacter clinical Foodborne illnesses | CDC". www.cdc.gov. Retrieved 2016-02-14.
- "Campylobacter Infections: Background, Pathophysiology, Epidemiology". 2019-02-02. Cite journal requires
|journal=(help) - Ryan, Kenneth James; Ray, C. George, eds. (2004). Sherris Medical Microbiology: An Introduction to Infectious Diseases (4th ed.). McGraw Hill. pp. 378–80. ISBN 978-0-8385-8529-0.
- Moore, John E.; Corcoran, Deborah; Dooley, James S.G.; Fanning, Séamus; Lucey, Brigid; Matsuda, Motoo; McDowell, David A.; Mégraud, Francis; Millar, B.; O'Mahony, Rebecca; O'Riordan, Lisa; O'Rourke, Michele; Rao, Juluri R.; Rooney, Paul J.; Sails, Andrew; Whyte, Paul (2005). "Campylobacter" (PDF). Veterinary Research. 36 (3): 351–82. doi:10.1051/vetres:2005012. PMID 15845230.
- Sauerwein, R. W.; Horrevorts, A. M.; Bisseling, J. (1993). "Septic abortion associated with Campylobacter fetus subspecies fetus infection: Case report and review of the literature". Infection. 21 (5): 331–3. doi:10.1007/BF01712458. PMID 8300253.
- Wang, Kun; Lu, Wenxin; Tu, Qichao; Ge, Yichen; He, Jinzhi; Zhou, Yu; Gou, Yaping; Nostrand, Joy D Van; Qin, Yujia; Li, Jiyao; Zhou, Jizhong; Li, Yan; Xiao, Liying; Zhou, Xuedong (10 March 2016). "Preliminary analysis of salivary microbiome and their potential roles in oral lichen planus". Scientific Reports. 6 (1): 22943. Bibcode:2016NatSR...622943W. doi:10.1038/srep22943. PMC 4785528. PMID 26961389.
- Crushell, Ellen; Harty, Sinead; Sharif, Farhana; Bourke, Billy (2004-01-01). "Enteric Campylobacter: Purging Its Secrets?". Pediatric Research. 55 (1): 3–12. doi:10.1203/01.PDR.0000099794.06260.71. ISSN 0031-3998. PMID 14605259.
- "CAMPYLOBACTER : Food Safety Watch". www.foodsafetywatch.org. Archived from the original on 2017-03-18. Retrieved 2017-03-17.
- Samie, A.; Obi, C.L.; Barrett, L.J.; Powell, S.M.; Guerrant, R.L. (2007). "Prevalence of Campylobacter species, Helicobacter pylori and Arcobacter species in stool samples from the Venda region, Limpopo, South Africa: Studies using molecular diagnostic methods". Journal of Infection. 54 (6): 558–66. doi:10.1016/j.jinf.2006.10.047. PMID 17145081.
- Condran, Gretchen A.; Murphy, Jennifer (2008). "Defining and Managing Infant Mortality: A Case Study of Philadelphia, 1870–1920". Social Science History. 32 (4): 473–513. doi:10.1215/01455532-2008-006.
- Skirrow, M. B. (1 November 2006). "John McFadyean and the Centenary of the First Isolation of Campylobacter Species". Clinical Infectious Diseases. 43 (9): 1213–1217. doi:10.1086/508201. PMID 17029145.
- Debruyne, Lies; Gevers, Dirk; Vandamme, Peter (2008). "Taxonomy of the Family Campylobacteraceae". In Nachamkin, Irving; Szymanski, Christine M.; Blaser, Martin J. (eds.). Campylobacter (3rd ed.). ASM Press. pp. 3–25. hdl:1854/LU-680725. ISBN 978-1-55581-437-3.
- Relman, David A.; Fouts, Derrick E; Mongodin, Emmanuel F; Mandrell, Robert E; Miller, William G; Rasko, David A; Ravel, Jacques; Brinkac, Lauren M; DeBoy, Robert T; Parker, Craig T; Daugherty, Sean C; Dodson, Robert J; Durkin, A. Scott; Madupu, Ramana; Sullivan, Steven A; Shetty, Jyoti U; Ayodeji, Mobolanle A; Shvartsbeyn, Alla; Schatz, Michael C; Badger, Jonathan H; Fraser, Claire M; Nelson, Karen E (2005). "Major Structural Differences and Novel Potential Virulence Mechanisms from the Genomes of Multiple Campylobacter Species". PLoS Biology. 3 (1): e15. doi:10.1371/journal.pbio.0030015. PMC 539331. PMID 15660156.
- Parkhill, J.; Wren, B. W.; Mungall, K.; Ketley, J. M.; Churcher, C.; Basham, D.; Chillingworth, T.; Davies, R. M.; Feltwell, T.; Holroyd, S.; Jagels, K.; Karlyshev, A. V.; Moule, S.; Pallen, M. J.; Penn, C. W.; Quail, M. A.; Rajandream, M-A.; Rutherford, K. M.; van Vliet, A. H. M.; Whitehead, S.; Barrell, B. G. (2000). "The genome sequence of the food-borne pathogen Campylobacter jejuni reveals hypervariable sequences". Nature. 403 (6770): 665–8. Bibcode:2000Natur.403..665P. doi:10.1038/35001088. PMID 10688204.
- Gupta, Radhey S (2006). "Molecular signatures (unique proteins and conserved indels) that are specific for the epsilon proteobacteria (Campylobacterales)". BMC Genomics. 7: 167. doi:10.1186/1471-2164-7-167. PMC 1557499. PMID 16817973.
- Grant, Christopher C. R.; Konkel, Michael E.; Cieplak, Witold; Tompkins, Lucy S. (1993). "Role of flagella in adherence, internalization, and translocation of Campylobacter jejuni in nonpolarized and polarized epithelial cell cultures". Infection and Immunity. 61 (5): 1764–71. PMC 280763. PMID 8478066.
- Firehammer, BD; Border, M (1968). "Isolation of temperate bacteriophages from Vibrio fetus". American Journal of Veterinary Research. 29 (11): 2229–35. PMID 5693467.
- Fletcher, R. D. (1965). "Activity and morphology of Vibrio coli phage". American Journal of Veterinary Research. 26 (111): 361–4.
- Fletcher, R. D.; Bertschinger, H. U. (2010). "A Method of Isolation ofVibrio colifrom Swine Fecal Material by Selective Filtration". Zentralblatt für Veterinärmedizin. Reihe B. 11 (6): 469–74. doi:10.1111/j.1439-0450.1964.tb01075.x.
- Connerton, P.L.; Timms, A.R.; Connerton, I.F. (2011). "Campylobacter bacteriophages and bacteriophage therapy". Journal of Applied Microbiology. 111 (2): 255–65. doi:10.1111/j.1365-2672.2011.05012.x. PMID 21447013.
- Zilbauer, Matthias; Dorrell, Nick; Wren, Brendan W.; Bajaj-Elliott, Mona (2008). "Campylobacter jejuni-mediated disease pathogenesis: an update". Transactions of the Royal Society of Tropical Medicine and Hygiene. 102 (2): 123–129. doi:10.1016/j.trstmh.2007.09.019. PMID 18023831.
- Humphrey, Tom; O'Brien, Sarah; Madsen, Mogens (2007). "Campylobacters as zoonotic pathogens: A food production perspective". International Journal of Food Microbiology. 117 (3): 237–57. doi:10.1016/j.ijfoodmicro.2007.01.006. PMID 17368847.
- "Infections from some foodborne germs increased, while others remained unchanged in 2012" (Press release). CDC. April 18, 2013. Retrieved October 22, 2015.
- "Infections from some foodborne germs increased, while others remained unchanged in 2012". Centers for Disease Control. April 18, 2013. Retrieved April 19, 2013.
- Jassim, S.S.; Malik, A.; Aldridge, A. (2011). "Small bowel perforation: an unusual cause". Grand Rounds. 11 (1): 17–9. doi:10.1102/1470-5206.2011.0006.
- Ternhag A, Asikainen T, Giesecke J, Ekdahl K (2007). "A meta-analysis on the effects of antibiotic treatment on duration of symptoms caused by infection with Campylobacter species". Clin Infect Dis. 44 (5): 696–700. doi:10.1086/509924. PMID 17278062.
- Vukelic, Dalibor; Trkulja, Vladimir; Salkovic-Petrisic, Melita (2010). "Single Oral Dose of Azithromycin Versus 5 Days of Oral Erythromycin or No Antibiotic in Treatment of Campylobacter Enterocolitis in Children: A Prospective Randomized Assessor-Blind Study". Journal of Pediatric Gastroenterology and Nutrition. 50 (4): 404–10. doi:10.1097/MPG.0b013e3181a87104. PMID 19881393.
- Gendrel, D.; Cohen, R. (2008). "Diarrhées bactériennes et antibiotiques : les recommandations européennes" [Bacterial diarrheas and antibiotics: European recommendations]. Archives de Pédiatrie (in French). 15 (Suppl 2): S93–6. doi:10.1016/S0929-693X(08)74223-4. PMID 19000862.
- Lehtopolku, M.; Nakari, U.-M.; Kotilainen, P.; Huovinen, P.; Siitonen, A.; Hakanen, A. J. (2010). "Antimicrobial Susceptibilities of Multidrug-Resistant Campylobacter jejuni and C. coli Strains: In Vitro Activities of 20 Antimicrobial Agents". Antimicrobial Agents and Chemotherapy. 54 (3): 1232–6. doi:10.1128/AAC.00898-09. PMC 2825995. PMID 20038624.
- "FSA warns that chicken bacteria could be next meat scandal". The Telegraph. January 23, 2013.
- "Don't wash raw chicken". Food Standards Agency.
- "Campylobacter survey: cumulative results from the full 12 months (Q1 – Q4)" (Press release). Food Standards Agency. May 28, 2015. Retrieved October 23, 2015.
- Williams, Aretha; Oyarzabal, Omar A (2012). "Prevalence of Campylobacter spp. in skinless, boneless retail broiler meat from 2005 through 2011 in Alabama, USA". BMC Microbiology. 12: 184. doi:10.1186/1471-2180-12-184. PMC 3490988. PMID 22920043.
- Food Safety and Inspection Service (April 24, 2015). "Quarterly Progress Report on Salmonella and Campylobacter: Testing of Selected Raw Meat and Poultry Products: Preliminary Results, July 2014 to September 2014". United States Department of Agriculture.
- "FoodNet Canada 2014 Short Report". Public Health Agency of Canada, FoodNet Canada. 2016-01-12. Retrieved 3 October 2016.
- "Woman died in Havelock North gastro outbreak". Stuff. 19 August 2016.
- "Govt rejects call for Hawke's Bay water emergency declaration". Radio New Zealand. 19 August 2016.
- "Fant samme bakterie i drikkevannet som hos sykehuspasienter fra Askøy". NRK. 11 June 2019.
External links
- Campylobacter genomes and related information at PATRIC, a Bioinformatics Resource Center funded by NIAID
- Campylobacter info from the CDC