We need you! Join our contributor community and become a WikEM editor through our open and transparent promotion process.
Difference between revisions of "Ecstasy (MDMA)"
From WikEM
(→Agitation) |
|||
| Line 2: | Line 2: | ||
==Background== | ==Background== | ||
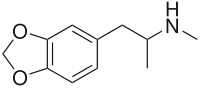
*3,4-methylenedioxymethamphetamine (MDMA) | *3,4-methylenedioxymethamphetamine (MDMA) | ||
| − | * | + | *Also known as: X, Molly, Skittles, Smartees, Beans |
| − | * | + | *Popular at "rave" parties and EDM festivals |
| − | + | *Causes catecholamine release, serotonin release, and inhibits serotonin re-uptake | |
*1-2mg/kg effective dose; onset 30min-1 hour, peak 4 hours, lasts 8-24 hours | *1-2mg/kg effective dose; onset 30min-1 hour, peak 4 hours, lasts 8-24 hours | ||
| − | * | + | **Typical tablets contain 50-100mg of MDMA |
==Clinical Features== | ==Clinical Features== | ||
| − | * | + | *Euphoria |
*[[altered mental status]] | *[[altered mental status]] | ||
| − | * | + | *Agitation |
| − | * | + | *Tachycardia, palpitations, hypertension |
*[[Serotonin Syndrome]] ([[altered mental status]], [[Hyperthermia]], rigidity, autonomic instability) | *[[Serotonin Syndrome]] ([[altered mental status]], [[Hyperthermia]], rigidity, autonomic instability) | ||
*rhabdomyolysis, myoglobinuria | *rhabdomyolysis, myoglobinuria | ||
| Line 25: | Line 25: | ||
*Hepatotoxicity<ref>Carvalho M, Pontes H, Remiao F, Bastos ML, Carvalho F. Mechanisms underlying the hepatotoxic effects of ecstasy. Curr Pharm Biotechnol. 2010;11(5):476-95</ref> | *Hepatotoxicity<ref>Carvalho M, Pontes H, Remiao F, Bastos ML, Carvalho F. Mechanisms underlying the hepatotoxic effects of ecstasy. Curr Pharm Biotechnol. 2010;11(5):476-95</ref> | ||
| − | == | + | ==Differential Diagnosis== |
| + | {{Sympathomimetic types}} | ||
| + | |||
| + | ==Evaluation== | ||
{{Hallucinogen workup}} | {{Hallucinogen workup}} | ||
| − | *Urine tox fails to detect unless large | + | *Urine tox fails to detect unless large doses |
**More usually positive test for amphetamines | **More usually positive test for amphetamines | ||
**Confirmation must use specialized lab tests (gas chromatography) | **Confirmation must use specialized lab tests (gas chromatography) | ||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
==Management== | ==Management== | ||
| Line 76: | Line 74: | ||
==Disposition== | ==Disposition== | ||
| − | * | + | *Consider discharge if all symptoms resolve and no complications noted |
| − | * | + | *Otherwise admit |
==References== | ==References== | ||
| − | <references /> | + | <references/> |
==See Also== | ==See Also== | ||
Revision as of 23:58, 9 May 2017
Contents
Background
- 3,4-methylenedioxymethamphetamine (MDMA)
- Also known as: X, Molly, Skittles, Smartees, Beans
- Popular at "rave" parties and EDM festivals
- Causes catecholamine release, serotonin release, and inhibits serotonin re-uptake
- 1-2mg/kg effective dose; onset 30min-1 hour, peak 4 hours, lasts 8-24 hours
- Typical tablets contain 50-100mg of MDMA
Clinical Features
- Euphoria
- altered mental status
- Agitation
- Tachycardia, palpitations, hypertension
- Serotonin Syndrome (altered mental status, Hyperthermia, rigidity, autonomic instability)
- rhabdomyolysis, myoglobinuria
- DIC
- GI symptoms
- Dehydration
- Bruxism (jaw clenching/grinding)
- Hyperthermia
- Hyponatremia (from sweat loss, free water intake, and SIADH-like effect) [1]
- Seizure
- Mydriasis
- Hepatotoxicity[2]
Differential Diagnosis
Sympathomimetics
- Cocaine
- Amphetamines
- Ketamine
- Ecstasy (MDMA)
- Synthetic cannabinoids
- Bath salts
Evaluation
- Urine pregnancy
- CBC, Metabolic panel, LFTs, coags, APAP level, ASA level
- Total CK level
- ECG
- UA
- Tox screen, blood alcohol
- Serum osmoles, urine Na (if Hyponatremia present)
- Head CT as indicated
- LP to rule out Meningitis if infectious symptoms and based on history and physical
- Urine tox fails to detect unless large doses
- More usually positive test for amphetamines
- Confirmation must use specialized lab tests (gas chromatography)
Management
Prehospital
- Primary focus should be on controlling agitation as well as ABCs
ABCs
- IV, O2, monitor
- Airway: Intubate if necessary
- Breathing: not expected to cause hypoxia, consider other dx or concurrent problem (aspiration PNA)
- Circulation: severe hypertension
- benzodiazepines first line
- Consider nitroprusside or phentolamine, avoid beta blockers (unopposed alpha stimulation)
Agitation
- Sedation with Benzodiazepines as needed
- Avoid Haldol, interferes with heat dissipation, may prolong QTc, may reduce seizure threshold
Seizure
- Benzodiazepines
- Phenobarbital (20mg/kg) or propofol as second line agents
- avoid dilantin
- manage airway as indicated
Seizure AND Hyponatremia
- Adults: 3% NS 100cc bolus over 10min; repeat after 10min x1 if no improvement[3]
- Each 100 ml will raise sodium by ~2 mmol/l
- In general, 200-400 mL of 3% NaCl is reasonable dose in most adult patients with severe symptomatic hyponatremia, which may be given IV over 1-2 hr until resolution of seizures.
- Pediatrics: 2 cc/kg of 3% over 10-60 minutes can be infused with a repeat of up to 3 times.[4]
- Goal should be to raise serum Na by 3-5 meq/L)
Hyponatremia
- Fluids restrict most patients, unless hypovolemic.
- Correct Na slowly: 0.5 meq/h; 10-12 meq/24h
Hyperthermia
- Ice packs, cold IVF,
- Rhabdomyolysis
- Foley, IVF, goal urine output > 2cc/kg
Gastrointestinal decontamination
- Activated charcoal for recent ingestion (< 1 hour)
- Patient must be protecting airway or intubated
Disposition
- Consider discharge if all symptoms resolve and no complications noted
- Otherwise admit
References
- ↑ Aitchison KJ, Tsapakis EM, Huezo-Diaz P, Kerwin RW, Forsling ML, Wolff K. Ecstasy (MDMA)-induced hyponatraemia is associated with genetic variants in CYP2D6 and COMT. J Psychopharmacol. 2012;26(3):408-18
- ↑ Carvalho M, Pontes H, Remiao F, Bastos ML, Carvalho F. Mechanisms underlying the hepatotoxic effects of ecstasy. Curr Pharm Biotechnol. 2010;11(5):476-95
- ↑ Spasovski et al. Clinical practice guideline on diagnosis and treatment of hyponatraemia. Nephrol Dial Transplant (2014) 0: 1–39. fulltext
- ↑ Moritz ML, Ayus JC. 100cc 3% sodium chloride bolus: a novel treatment for hyponatremic encephalopathy. Metab Brain Dis. 2010 Mar; 25(1): 91-6.