 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Progress Toward Poliomyelitis Eradication -- Myanmar, 1996-1999Myanmar borders polio-free countries (China, Laos, and Thailand) and countries with widespread poliovirus transmission (India and Bangladesh). Myanmar began to intensify its efforts toward polio eradication in 1996, when National Immunization Days (NIDs)* were initiated. That year, wild polioviruses (one type 1 virus and two type 3 viruses) were isolated from Myanmar children with acute poliomyelitis seeking care in Yunnan Province, China. The importation of poliovirus from Myanmar into China stimulated the establishment of surveillance for acute flaccid paralysis (AFP) in 1996 and discussions between Myanmar and China on cross-border management of poliomyelitis eradication. This report summarizes polio eradication efforts in Myanmar, which focus primarily on supplemental vaccination activities and AFP surveillance. Routine Vaccination The national Expanded Program on Immunization was initiated in April 1978, and activities were accelerated in 1986 to meet the goal of universal childhood vaccination in 1990. Reported routine coverage of infants with three doses of oral poliovirus vaccine (OPV3) in 1995 was 84% and in 1997 was 90%; however, survey** results indicated that coverage was 75% and 82%, respectively (1). Results of the 1997 survey revealed large differences within states/divisions; lowest OPV3 coverage was observed in rural Myanmar (border and hill areas): Shan East (50%), Kayah (52%), Chin (58%), Kayin (62%), Kokang/Wa in Shan North (45%), and Kabaw/Naga in Sagaing (65%). Another survey** in Rakhine showed OPV3 coverage in 1996 to be 19% in Maungdaw and 30% in Buthidaung (compared with reported coverage of 78.9% and 75.2%, respectively) (2). These townships share a border with Bangladesh. NIDs and Supplemental ("Mopping-Up") Vaccination Activities NIDs were first conducted in February and March 1996, and since then Myanmar has organized two rounds of NIDs (one day each) in December and January during 1996-1999, targeting all children aged less than 5 years. Reported coverage during those years has been greater than 95%. However, no post-NID coverage surveys have been conducted. Since the winter of 1996, NIDs in Myanmar have been synchronized with those in neighboring countries, including Bangladesh, China, India, and Thailand. The fifth NIDs will be conducted on December 12, 1999, and January 16, 2000. Mopping-up vaccination campaigns*** are being planned for October and November 1999, targeting 917,000 children in high-risk areas (those along the border with India and Bangladesh, with recent wild virus circulation or known low vaccination coverage, or with minorities and migrating groups). These campaigns will be carried out by mobile teams over approximately 5 days, focusing on reaching previously unvaccinated children by going house to house. Volunteers also will collect information on the number of children who have never received OPV ("zero dose" children) and ascertain recent cases of paralysis. AFP Surveillance In 1996, when AFP became a reportable condition in Myanmar, intensive training and advocacy sessions were organized for clinicians and public health staff. Reporting rates for AFP and nonpolio AFP improved from 1997 to 1998, from 0.75 to 0.91 per 100,000 children aged less than 15 years (Table 1). Approximately 2000 health facilities (health centers and hospitals) participate in a routine reporting system of "zero-case reporting," submitting weekly reports, even if no cases are seen. In addition, surveillance staff make weekly visits to 30 large hospitals to search actively for AFP cases. Since early 1999, the AFP surveillance system also has been used for reporting of measles and neonatal tetanus cases. Of 92 AFP cases reported during January 1-October 15, 1999, 91 (99%) had at least one stool specimen taken, and 62 (67%) had two specimens taken within 14 days after onset of paralysis (i.e., "adequate specimens"). Of 37 (40%) persons with AFP for whom follow-up results were available, three (8%) had died, one (3%) was lost to follow-up, 20 (54%) had no residual paralysis, and 13 (35%) had residual paralysis. Myanmar classifies AFP cases using the clinical classification scheme****. In 1999, wild poliovirus type 1 was isolated from four persons with AFP (Figure 1), all of whom were children among the Muslim minority living in Rakhine state, near the border with Bangladesh. Stool specimens from persons with AFP are processed at the national health laboratories in Yangoon, which have been accredited provisionally as a National Polio Laboratory. Intra-typic differentiation is performed by the Regional Reference Laboratory at the National Institute of Health in Bangkok, Thailand. A national certification committee has been established and monitors progress in the polio eradication program. Reported by: Expanded Program on Immunization, Ministry of Health, Yangoon, Myanmar. Country Office, World Health Organization, Yangoon, Myanmar; Regional Office for South-East Asia, World Health Organization, New Delhi, India; Vaccines and Biologicals Department, World Health Organization, Geneva, Switzerland. Respiratory and Enteric Viruses Br, Div of Viral and Rickettsial Diseases, National Center for Infectious Diseases; Vaccine Preventable Disease Eradication Div, National Immunization Program, CDC. Editorial Note:In 1999, Myanmar, situated between countries with endemic polio and polio-free countries, has confirmed four cases of polio based on isolation of wild poliovirus type 1. This is the first evidence of ongoing transmission of wild poliovirus since 1996. All AFP cases with wild poliovirus isolation occurred in persons who resided in areas adjacent to the Bangladesh border, illustrating the importance of border areas in polio eradication activities and the continuing vulnerability of countries to a resurgence of polio unless eradication strategies are fully implemented and sustained. Vaccination coverage in Myanmar is not uniform across the country. Border and mountain areas with difficult access are underserved, allowing pockets of low coverage to develop. Low coverage in these areas can be explained by difficulties in access, cultural differences between health staff and local sub-populations, and lack of awareness among the population. Children who have not been reached by routine services also are likely to be missed during NIDs. The planned mopping-up operations in high-risk areas are an appropriate response to the situation provided that these supplemental campaigns succeed in reaching all children, including those missed by NIDs. AFP surveillance in Myanmar has not yet reached the level that would define the extent of poliovirus transmission. The nonpolio AFP rate approached the target of one case per 100,000 children aged less than 15 years in 1998, but declined in 1999. The rate of collection of two stool specimens in 14 days of onset of paralysis also is lower than the 80% target. Although mopping-up campaigns and high-quality NIDs are needed to eliminate the remaining foci of poliovirus circulation, AFP surveillance needs to be strengthened to support these activities. Ongoing advocacy, supervision, feedback, and monitoring are needed to sustain the momentum achieved since 1997. The successful approach taken by India (3) (i.e., the establishment of a team dedicated to AFP surveillance), may provide some guidance to improve AFP surveillance in Myanmar. With fewer than 16 months remaining to reach the target of polio eradication, Myanmar is stepping up efforts to vaccinate previously unreached children. This effort must be supported by high-quality surveillance. The priorities for the Myanmar program***** for the next year include 1) continuing to improve the quality of the upcoming NIDs in 1999 and 2000; 2) vaccinating a high proportion of previously unreached children during the mopping-up campaigns this fall; and 3) improving the sensitivity of AFP surveillance rapidly to identify high-risk areas for special programmatic action and, eventually, to meet the certification requirements. Further progress in these priority areas should enable Myanmar to reach the polio eradication target. References
* Nationwide mass campaigns over a short period (days to weeks), in which two doses of oral poliovirus vaccine are administered to all children in the target age group (usually aged less than 5 years), regardless of vaccination history, with an interval of 4-6 weeks between doses. ** Reported coverage may be affected by uncertainties of the numerator (doses of vaccine administered) and denominator (actual target population). Because these uncertainties do not affect population-based surveys, data from such surveys usually provide more precise estimates of the actual vaccination coverage. *** Focal mass campaigns in high-risk areas during a short period (days to weeks) in which two doses of oral poliovirus vaccine are administered during house-to-house visits to all children in the target age groups, regardless of vaccination history, with an interval of 4-6 weeks between doses. **** An AFP case is confirmed as polio if wild poliovirus was isolated from stool specimens; in the absence of wild poliovirus isolation, the following criteria confirm a case of polio: 1) residual paralysis at follow-up examination; 2) lost to follow-up; and 3) died. ***** Polio eradication in Myanmar is supported by the national government and a coalition of organizations and governments, including WHO, UNICEF, Rotary International, and Japan. Table 1 Note: To print large tables and graphs users may have to change their printer settings to landscape and use a small font size. TABLE 1. Acute flaccid paralysis (AFP) and confirmed poliomyelitis cases -- Myanmar, 1995-1999
* Per 100,000 children aged <15 years. Return to top. Figure 1 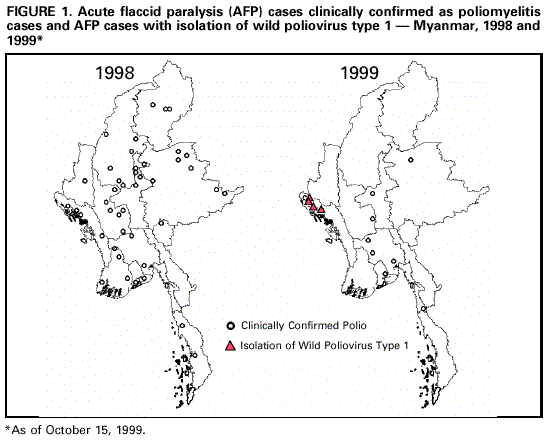 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 10/28/1999 |
||||||||||||||||||||||||||||||||||||||||||||
This page last reviewed 5/2/01
|