Trachea
The trachea, colloquially called the windpipe, is a cartilaginous tube that connects the pharynx and larynx to the lungs, allowing the passage of air, and so is present in almost all air-breathing animals with lungs. The trachea extends from the larynx and branches into the two primary bronchi. At the top of the trachea the cricoid cartilage attaches it to the larynx. This is the only complete tracheal ring, the others being incomplete rings of reinforcing cartilage. The trachealis muscle joins the ends of the rings and these are joined vertically by bands of fibrous connective tissue – the annular ligaments of trachea. The epiglottis closes the opening to the larynx during swallowing.
| Trachea | |
|---|---|
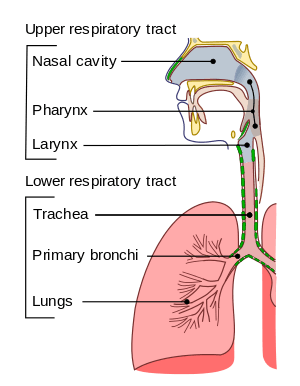 Conducting passages. | |
| Details | |
| Pronunciation | /trəˈkiːə, ˈtreɪkɪə/[1] |
| Artery | tracheal branches of inferior thyroid artery |
| Vein | brachiocephalic vein, azygos vein accessory hemiazygos vein |
| Identifiers | |
| Latin | Trachea |
| MeSH | D014132 |
| TA | A06.3.01.001 |
| FMA | 7394 |
| Anatomical terminology | |
The trachea develops in the second month of development. It is lined with an epithelium that has goblet cells which produce protective mucins (see Respiratory epithelium). An inflammatory condition, also involving the larynx and bronchi, called croup can result in a barking cough. A tracheotomy is often performed for ventilation in surgical operations where needed. Intubation is also carried out for the same reason by the inserting of a tube into the trachea. From 2008, operations have experimentally transplanted a windpipe grown by stem cells, and synthetic windpipes; however, a successful method for this method of transplant does not currently exist and development of such a method remains theoretically daunting.[2][3]
The word "trachea" is used to define a very different organ in invertebrates than in vertebrates. Insects have an open respiratory system made up of spiracles, tracheae, and tracheoles to transport metabolic gases to and from tissues.
Structure
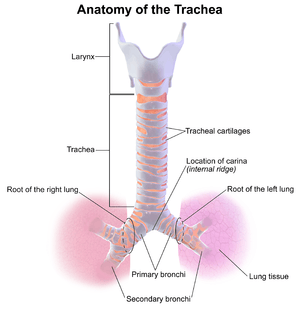
An adult's trachea has an inner diameter of about 1.5 to 2 centimetres (0.59 to 0.79 in) and a length of about 10 to 11 centimetres (3.9 to 4.3 in); wider in males than females.[4] It begins at the bottom of the larynx, and ends at the carina, the point where the trachea branches into left and right main bronchi.[4]The trachea is surrounded by 16-20 rings of hyaline cartilage; these 'rings' are incomplete and C-shaped.[4]
Position
It begins at the bottom of the larynx, and ends at the carina, the point where the trachea branches into left and right main bronchi.[4] The trachea begins level with the sixth cervical vertebra (C6) and the carina is found at the level of the sixth thoracic vertebra (T6),[4]opposite the sternal angle and can be positioned up to two vertebrae lower or higher, depending on breathing.
The trachea passes by many structures of the neck and thorax along its course. In front of the upper trachea lies connective tissue and skin.[4]Several other structures pass or sit over it; the jugular arch, which joins the two anterior jugular veins, sits in front of the upper part of the trachea. The sternohyoid and sternothyroid muscles stretch along its length, and the thyroid gland sits below this; with the isthmus of the gland overlying the second to fourth rings, with the lobes of the thyroid stretching to the level of the fifth or sixth cartilage.[4] The vessels of the thyroid sit adjacent to the thyroid isthmus on the trachea; the superior thyroid arteries join just above it, and the inferior thyroid veins below it.[4] In front of the lower trachea lies the manubrium of the sternum, the remnants of the thymus in adults; to the front left the large blood vessels the aortic arch and its branches the left common carotid artery and the brachiocephalic trunk; and the left brachiocephalic vein. The deep cardiac plexus and lymph nodes are also positioned in front of the lower trachea.[4]
Behind the trachea, along its length, sits the oesophagus, followed by connective tissue and the vertebral column.[4] To its sides run the carotid arteries and inferior thyroid arteries; and to its sides on its back surface run the recurrent laryngeal nerves in the upper trachea, and the vagus nerves in the lower trachea.[4]
The trachealis muscle connects the ends of the incomplete rings and contracts during coughing, reducing the size of the lumen of the trachea to increase the rate of air flow.[5] The esophagus lies posteriorly to the trachea, adjoining along the tracheoesophageal stripe. Circular horizontal bands of fibrous tissue called the annular ligaments of trachea join the tracheal rings together. The cartilaginous rings are incomplete to allow the trachea to collapse slightly so that food can pass down the esophagus. A flap-like epiglottis closes the opening to the larynx during swallowing to prevent swallowed matter from entering the trachea.
- The sternohyoid and sternothyroid muscles lie on top of the upper part of the trachea
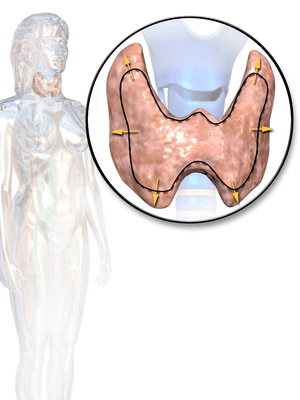 The thyroid gland also lies on top of the trachea, and lies below the cricoid cartilage. The isthmus of the thyroid, which connects both wings, lies directly in front, whereas the wings lie on the front and stretch to the side.
The thyroid gland also lies on top of the trachea, and lies below the cricoid cartilage. The isthmus of the thyroid, which connects both wings, lies directly in front, whereas the wings lie on the front and stretch to the side.
Blood and lymphatic supply
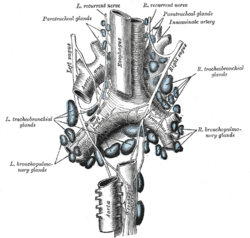
The trachea mostly receives and drains blood through the inferior thyroid arteries and veins.[4] The arteries arise just below the isthmus of the thyroid, which sits atop the trachea. These arteries join (anastamoses) with ascending branches of the bronchial arteries to supply blood to the trachea.[4] The lymphatic vessels of the trachea drain into the pretracheal nodes that lie in front of the trachea, and paratracheal lymph nodes that lie beside it.[4]
Development
In the fourth week of development of the human embryo as the respiratory bud grows, the trachea separates from the foregut through the formation of tracheoesophageal ridges which fuse to form the tracheoesophageal septum and this separates the future trachea from the oesophagus and divides the foregut tube into the laryngotracheal tube.[6] By the start of the fifth week, the left and right main bronchi have begin to form, initially as buds at the terminal end of the treachea.[6]
The trachea is no more than 4mm diameter during the first year of life, expanding to its adult diameter by late childhood. The trachea is of more variable length and site in relation to its surrounding structures in children.[4]
Microanatomy
The trachea is lined with a layer of pseudostratified ciliated columnar epithelium. The epithelium contains goblet cells, which are glandular, modified simple columnar epithelial cells that produce mucins, the main component of mucus. Mucus helps to moisten and protect the airways.[7] Mucus lines the ciliated cells of the trachea to trap inhaled foreign particles that the cilia then waft upward toward the larynx and then the pharynx where it can be either swallowed into the stomach or expelled as phlegm. This self-clearing mechanism is termed mucociliary clearance.[8]
The trachea is surrounded by 16-20 rings of hyaline cartilage; these 'rings' are incomplete and C-shaped.[4]Two or more of the cartilages often unite, partially or completely, and they are sometimes bifurcated at their extremities. The rings are generally highly elastic but they may calcify with age.
 Cross-section
Cross-section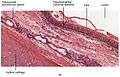 Cross-section of the trachea, with pseudostratified ciliated columnar epithelium and goblet cells labelled
Cross-section of the trachea, with pseudostratified ciliated columnar epithelium and goblet cells labelled- Magnified cross-section of the cartilage of the trachea.
Clinical significance
Inflammation
Inflammation of the trachea is known as tracheitis. It can also occur with inflammation of the larynx and bronchi, known as croup.[9] It can be caused by viruses and bacteria, with typical bacterial causes including staphylococcus aureus, haemophilus influenzae, streptococcus pneumonia, and pseudomonas aeruginosa.[10] Bacterial tracheitis occurs almost entirely in children.[9]
A person affected with bacterial tracheitis may start with symptoms that suggest an upper respiratory tract infection; this may include a cough, sore throat, or coryzal symptoms (such as a runny nose). Fevers may develop. Swelling of the airway may eventually progress to airway obstruction; when the airway is narrowed, this may result in a hoarse breathing sound called stridor.[9]
Unfortunately, up to 80% of people affected by tracheitis require intubation, and treatment may include endoscopy for the purposes of acquiring microbiological specimens for culture and sensitivity, as well as removal (debridement) of any dead tissue associated with the infection. Treatment of the underlying cause usually involves antibiotics.[9]
Narrowing
A trachea may be narrowed of compressed, usually a result of enlarged nearby lymph nodes; cancers of the trachea or nearby structures; large thyroid goitres; or rarely as a result of other processes such as unusually swollen blood vessels.[11] Scarring from tracheobronchial injury or intubation; or inflammation associated with granulomatosis with polyangiitis may also cause a narrowing of the trachea (tracheal stenosis.[11] Obstruction invariably causes a harsh breathing sound known as stridor.[11] A camera inserted via the mouth down into the trachea, called bronchoscopy, may be performed to investigate the cause of an obstruction.[11]
Management of obstructions depends on the cause. Obstructions as a result of malignancy may be managed with surgery, chemotherapy or radiotherapy.[11] A stent may be inserted over the obstruction. Benign lesions, such as narrowing resulting from scarring, are likely to be surgically excised.[11]
Intubation
Tracheal intubation refers to the insertion of a catheter down the trachea. This procedure is commonly performed during surgery, in order to ensure a person receives enough oxygen when sedated. The catheter is connected to a machine that monitors the airflow, oxygenation and several other metrics. This is often one of the responsibilities of an anesthetist during surgery. The epiglottic vallecula is an important anatomical landmark for carrying out this procedure.
In an emergency, or when tracheal intubation is deemed impossible, a tracheotomy is often performed to insert a tube for ventilation, usually when needed for particular types of surgery to be carried out so that the airway can be kept open. The provision of the opening via a tracheotomy is called a tracheostomy.[12] Another less invasive method is used when a procedure can be carried out more quickly, or in an emergency situation, and this is a cricothyrotomy.
Congenital disorders
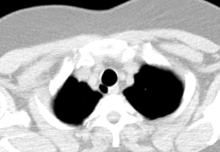
Tracheal agenesis[13] is a rare birth defect in which the trachea fails to develop. The defect is usually fatal though sometimes surgical intervention has been successful.
A tracheoesophageal fistula is a congenital defect in which the trachea and esophagus are abnormally connected (a fistula). This is because of abnormalities in the separation between the trachea and oesophagus during development.[6] This occurs in approximately 1 in 3000 births, and the most common abnormalities is a separation of the upper and lower ends of the oesophagus, with the upper end finishing in a closed pouch.[6] Other abnormalities may associated with this, including cardiac abnormalities, or VACTERL syndrome.[6] Such fistulas may be detected before a baby is born because of excess amniotic fluid; after birth, they are often associated with pneumonitis and pneumonia because of aspiration of food contents.[6] Congenital fistulas are often treated by surgical repair.[11] In adults, fistulas may occur because of erosion into the trachea from nearby malignant tumours, which erode into both the trachea and the oesophagus. Initially, these often result in coughing from swallowed contents of the oesophagus that are aspirated through the trachea, often progressing to fatal pneumonia; unfortunately there is rarely a curative treatment.[11] A tracheo-oesophageal puncture is a surgically created hole between the trachea and the esophagus in a person who has had a total laryngectomy, (removal of larynx). The purpose of the puncture is to restore a person's ability to speak after the vocal cords have been removed.
Sometimes as an anatomical variation one or more of the tracheal rings are completely formed. These O rings are smaller than the normal C-shaped rings and can cause narrowing of the trachea, resulting in breathing difficulties. An operation called a slide tracheoplasty can open up the rings and rejoin them as wider rings, shortening the length of the trachea.[14] Slide tracheoplasty is said to be the best option in treating tracheal stenosis.[15]
Mounier-Kuhn syndrome is a very rare congenital disorder of an abnormally enlarged trachea.
Other
- Tracheomalacia (weakening of the tracheal cartilage)
- Tracheal collapse (in dogs)
Other animals
Allowing for variations in the length of the neck, the trachea in other mammals is, in general, similar to that in humans. Generally, it is also similar to the reptilian trachea.[16]
Vertebrates
In birds, the trachea runs from the pharynx to the syrinx, from which the primary bronchi diverge. Swans have an unusually elongated trachea, part of which is coiled beneath the sternum; this may act as a resonator to amplify sound. In some birds, the tracheal rings are complete, and may even be ossified.[16]
In amphibians, the trachea is normally extremely short, and leads directly into the lungs, without clear primary bronchi. A longer trachea is, however, found in some long-necked salamanders, and in caecilians. While there are irregular cartilagenous nodules on the amphibian trachea, these do not form the rings found in amniotes.[16]
The only vertebrates to have lungs, but no trachea, are the lungfish and the Polypterus, in which the lungs arise directly from the pharynx.[16]
Invertebrates

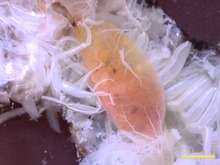
The word "trachea" is used to define a very different organ in invertebrates than in vertebrates. Insects have an open respiratory system made up of spiracles, tracheae, and tracheoles to transport metabolic gases to and from tissues.[17] The distribution of spiracles can vary greatly among the many orders of insects, but in general each segment of the body can have only one pair of spiracles, each of which connects to an atrium and has a relatively large tracheal tube behind it. The tracheae are invaginations of the cuticular exoskeleton that branch (anastomose) throughout the body with diameters from only a few micrometres up to 0.8 mm. Diffusion of oxygen and carbon dioxide takes place across the walls of the smallest tubes, called tracheoles, which penetrate tissues and even indent individual cells.[18] Gas may be conducted through the respiratory system by means of active ventilation or passive diffusion. Unlike vertebrates, insects do not generally carry oxygen in their haemolymph.[19] This is one of the factors that may limit their size.
A tracheal tube may contain ridge-like circumferential rings of taenidia in various geometries such as loops or helices. Taenidia provide strength and flexibility to the trachea. In the head, thorax, or abdomen, tracheae may also be connected to air sacs. Many insects, such as grasshoppers and bees, which actively pump the air sacs in their abdomen, are able to control the flow of air through their body. In some aquatic insects, the tracheae exchange gas through the body wall directly, in the form of a gill, or function essentially as normal, via a plastron. Note that despite being internal, the tracheae of arthropods are lined with cuticular tissue and are shed during moulting (ecdysis).[18]
Bioengineering and prosthesis
In 2008, a Colombian woman, Claudia Castillo (30), received a trachea transplant using her own stem cells.[20]
Between 2011 and 2014 Paolo Macchiarini of the Karolinska University Hospital performed eight operations in which he generated an artificial trachea from a person's stem cells; four of them at Karolinska, three in Russia, and one in Illinois.[2] In January 2016 the Swedish television station Sveriges Television broadcast a three part documentary about Macchiarini that suggested that Macchiarini did not obtain informed consent from these people, six of whom died.[2] Macchiraini had been a "media darling" and had been seen as a pioneer in the field.[2] In February 2016 Karolinska announced it would not renew his contract when it expired in November 2016 and that it would open an investigation of Macchiarini's work and publications.[2]
Several bioengineering approaches have been tested to repair and replace the trachea, indicating extraordinary difficulties in a successful graft due. A 2016 article cited the tremendous difficulties of tracheal revascularization as a major challenge to any form of tracheal replacement. The study also notes that on top of the revascularization issue, there is no evidence that using bone-marrow stem-cells on a de-cellularized native trachea or synthetic scaffold will induce airway tissue regeneration, and such a method remains hypothetical.[3]
Additional images
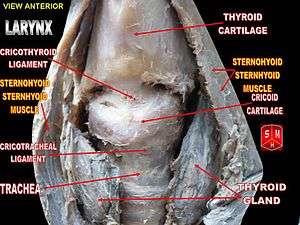 Trachea.
Trachea.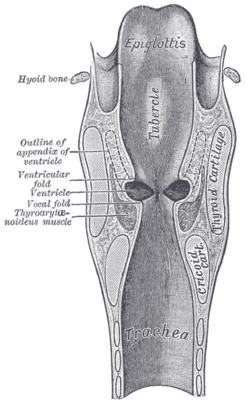 Coronal section of larynx and upper part of trachea.
Coronal section of larynx and upper part of trachea.
References
- "Trachea | Definition of Trachea by Lexico". Lexico Dictionaries | English. Retrieved 27 October 2019.
- "Karolinska Institute has 'lost confidence' in Paolo Macchiarini, says it won't renew his contract". KI. 4 February 2016. Retrieved 7 February 2016.
- Delaere, P; Van Raemdonck, D (March 2016). "Tracheal replacement". Journal of Thoracic Disease. 8 (Suppl 2): S186–96. doi:10.3978/j.issn.2072-1439.2016.01.85. PMC 4775267. PMID 26981270.
- Standring, Susan, ed. (2016). "Trachea and bronchi". Gray's anatomy : the anatomical basis of clinical practice (41st ed.). Philadelphia. pp. 965–969. ISBN 9780702052309. OCLC 920806541.
- Ross, Michael. Histology a text and atlas (5th ed.). Wojciech Pawlina. p. 617.
- Sadley, TW (2019). Langman's medical embryology (14th ed.). Philadelphia: Wolters Kluwer. pp. 223=229. ISBN 9781496383907.
- Mescher AL, "Chapter 17. The Respiratory System" (Chapter). Mescher AL: Junqueira's Basic Histology: Text & Atlas, 12e: "Archived copy". Archived from the original on 3 June 2013. Retrieved 24 February 2015.CS1 maint: archived copy as title (link).
- Antunes, MB; Cohen, NA (February 2007). "Mucociliary clearance—a critical upper airway host defense mechanism and methods of assessment". Current Opinion in Allergy and Clinical Immunology. 7 (1): 5–10. doi:10.1097/aci.0b013e3280114eef. PMID 17218804.
- Kuo, Connie Y.; Parikh, Sanjay R. (2014). "Bacterial Tracheitis". Pediatrics in Review. 35 (11): 497–499. doi:10.1542/pir.35-11-497. ISSN 0191-9601.
- Hopkins, Brandon S.; Johnson, Kaalan E.; Ksiazek, Jeff M.; Sun, Gordon; Greinwald, John H.; Rutter, Michael (2010). "H1N1 influenza A presenting as bacterial tracheitis". Otolaryngology–Head and Neck Surgery. 142 (4): 612–614. doi:10.1016/j.otohns.2010.01.005. ISSN 0194-5998.
- Ralston, Stuart H.; Penman, Ian D.; Strachan, Mark W.; Hobson, Richard P. (eds.) (2018). Davidson's principles and practice of medicine (23rd ed.). Elsevier. ISBN 978-0-7020-7028-0.CS1 maint: extra text: authors list (link)
- Molnar, Heather. "Types of Tracheostomy Tubes".
- Chiu, T.; Cuevas, D.; Cuevas, L.; Monteiro, C. (1990). "Tracheal agenesis". Southern Medical Journal. 83 (8): 925–930. doi:10.1097/00007611-199008000-00018. PMID 2200137.
- "Slide tracheoplasty". Retrieved 2 October 2015.
- Xue, B; Liang, B; Wang, S; Zhu, L; Lu, Z; Xu, Z (January 2015). "One-stage surgical correction of congenital tracheal stenosis complicated with congenital heart disease in infants and young children". Journal of Cardiac Surgery. 30 (1): 97–103. doi:10.1111/jocs.12418. PMID 25109422.
- Romer, Alfred Sherwood; Parsons, Thomas S. (1977). The Vertebrate Body. Philadelphia, PA: Holt-Saunders International. pp. 336–337. ISBN 978-0-03-910284-5.
- Wasserthal, Lutz T. (1998). Chapter 25: The Open Hemolymph System of Holometabola and Its Relation to the Tracheal Space. In "Microscopic Anatomy of Invertebrates". Wiley-Liss, Inc. ISBN 0-471-15955-7.
- Triplehorn, Charles (2005). Borror and DeLong's introduction to the study of insects. Johnson, Norman F., Borror, Donald J. (7th ed.). Belmont, CA: Thompson Brooks/Cole. pp. 28–29. ISBN 978-0030968358. OCLC 55793895.
- Westneat, Mark W.; Betz, Oliver; Blob, Richard W.; Fezzaa, Kamel; Cooper, James W.; Lee, Wah-Keat (January 2003). "Tracheal Respiration in Insects Visualized with Synchrotron X-ray Imaging". Science. 299 (5606): 558–560. doi:10.1126/science.1078008. PMID 12543973.
- "The top health stories of 2008 - CNN.com". CNN. 26 December 2008. Retrieved 27 May 2010.