Dermis
The dermis or corium is a layer of skin between the epidermis (with which it makes up the cutis) and subcutaneous tissues, that primarily consists of dense irregular connective tissue and cushions the body from stress and strain. It is divided into two layers, the superficial area adjacent to the epidermis called the papillary region and a deep thicker area known as the reticular dermis.[1] The dermis is tightly connected to the epidermis through a basement membrane. Structural components of the dermis are collagen, elastic fibers, and extrafibrillar matrix.[2] It also contains mechanoreceptors that provide the sense of touch and thermoreceptors that provide the sense of heat. In addition, hair follicles, sweat glands, sebaceous glands (oil glands), apocrine glands, lymphatic vessels, nerves and blood vessels are present in the dermis. Those blood vessels provide nourishment and waste removal for both dermal and epidermal cells.
| Dermis | |
|---|---|
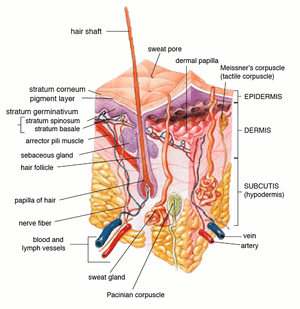 Cross-section of human skin | |
Cross section of skin under the microscope | |
| Details | |
| Part of | Skin |
| Identifiers | |
| MeSH | D020405 |
| TA | A16.0.00.010 |
| TH | H3.12.00.1.03001 |
| FMA | 70323 |
| Anatomical terminology | |
Structure
The dermis is composed of three major types of cells:[3] fibroblasts, macrophages, and mast cells.
Apart from these cells, the dermis is also composed of matrix components such as collagen (which provides strength), elastin (which provides elasticity), and extrafibrillar matrix, an extracellular gel-like substance primarily composed of glycosaminoglycans (most notably hyaluronan), proteoglycans, and glycoproteins.[3]
Layers
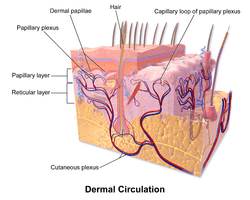
Papillary dermis
The papillary dermis is the uppermost layer of the dermis. It intertwines with the rete ridges of the epidermis and is composed of fine and loosely arranged collagen fibers.[2]
The papillary region is composed of loose areolar connective tissue. This is named for its fingerlike projections called papillae, that extend toward the epidermis and contain either terminal networks of blood capillaries or tactile Meissner's corpuscles.[4]
Reticular dermis
The reticular dermis is the lower layer of the dermis, found under the papillary dermis, composed of dense irregular connective tissue featuring densely packed collagen fibers. It is the primary location of dermal elastic fibers.[2]
The reticular region is usually much thicker than the overlying papillary dermis. It receives its name from the dense concentration of collagenous, elastic, and reticular fibers that weave throughout it. These protein fibers give the dermis its properties of strength, extensibility, and elasticity. Within the reticular region are the roots of the hair, sebaceous glands, sweat glands, receptors, nails, and blood vessels. The orientation of collagen fibers within the reticular dermis creates lines of tension called Langer's lines, which are of some relevance in surgery and wound healing.[5]
Dermal papillae
| Dermal papillae | |
|---|---|
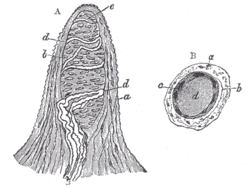 Papilla of the hand, treated with acetic acid. Magnified 350 times. A. Side view of a papilla of the hand. a. Cortical layer. b. Tactile corpuscle. c. Small nerve of the papilla, with neurolemma. d. Its two nervous fibers running in spiral coils around the tactile corpuscle. e. Apparent termination of one of these fibers. B. Tactile papilla seen from above so as to show its transverse section. a. Cortical layer. b. Nerve fiber. c. Outer layer of the tactile body, with nuclei. d. Clear interior substance. | |
| Details | |
| Identifiers | |
| Latin | papillae dermis |
| MeSH | D020405 |
| TA | A16.0.00.010 |
| TH | H3.12.00.1.03001 |
| FMA | 70323 |
| Anatomical terminology | |
The dermal papillae (DP) (singular papilla, diminutive of Latin papula, 'pimple') are small, nipple-like extensions (or interdigitations) of the dermis into the epidermis. At the surface of the skin in hands and feet, they appear as epidermal or papillary ridges (colloquially known as fingerprints).
Blood vessels in the dermal papillae nourish all hair follicles and bring nutrients and oxygen to the lower layers of epidermal cells. The pattern of ridges they produce in hands and feet are partly genetically determined features that develop before birth. They remain substantially unaltered (except in size) throughout life, and therefore determine the patterns of fingerprints, making them useful in certain functions of personal identification. [6]
The dermal papillae are part of the uppermost layer of the dermis, the papillary dermis, and the ridges they form greatly increase the surface area between the dermis and epidermis. Because the main function of the dermis is to support the epidermis, this greatly increases the exchange of oxygen, nutrients, and waste products between these two layers. Additionally, the increase in surface area prevents the dermal and epidermal layers from separating from each other by strengthening the junction between them. With age, the papillae tend to flatten and sometimes increase in number. [7]
Dermal papillae also play a pivotal role in hair formation, growth and cycling. [8]
In mucous membranes, the equivalent structures to dermal papillae are generally termed "connective tissue papillae", which interdigitate with the rete pegs of the superficial epithelium.
See also
- List of cutaneous conditions
- Epidermis
- Subcutaneous layer
References
- James, William; Berger, Timothy; Elston, Dirk (2005). Andrews' Diseases of the Skin: Clinical Dermatology (10th ed.). Saunders. Pages 1, 11–12. ISBN 0-7216-2921-0.
- Marks, James G; Miller, Jeffery (2006). Lookingbill and Marks' Principles of Dermatology (4th ed.). Elsevier Inc. Page 8–9. ISBN 1-4160-3185-5.
- malvi (4 March 2011). "The Ageing Skin - Part 1 - Structure of Skin and Introduction - Articles". PharmaXChange.info.
- http://microvet.arizona.edu/Courses/vsc422/secure/VSC422AppledHistologyLabHandout.pdf%5B%5D
- Ross M, Pawlina W (2011). Histology: A Text and Atlas (6th ed.). Lippincott Williams & Wilkins. p. 498. ISBN 978-0-7817-7200-6.
- "Dermal papillae". Probert Encyclopaedia. Archived from the original on 2011-06-08. Retrieved February 2010. Check date values in:
|accessdate=(help) - "Friction Skin". Ridges and Furrows. Retrieved February 2010. Check date values in:
|accessdate=(help) - Lin, Chang-min; et al. (October 2008). "Microencapsulated human hair dermal papilla cells: a substitute for dermal papilla?". Archives of Dermatological Research. Springer. 300 (9): 531–535. doi:10.1007/s00403-008-0852-3. PMID 18418617.
-solution.jpg)

