Lipedema
Lipedema is a disorder where there is enlargement of both legs due to deposits of fat under the skin.[1] Typically it gets worse over time, pain may be present, and sufferers bruise easily.[1] In severe cases the trunk and upper body may be involved.[1] Lipedema is commonly misdiagnosed.[2]
| Lipedema | |
|---|---|
| Other names | Lipoedema, lipödem, lipalgia, adiposalgia, adipoalgesia, adiposis dolorosa, lipomatosis dolorosa of the legs, lipohypertrophy dolorosa, painful column leg, painful lipedema syndrome |
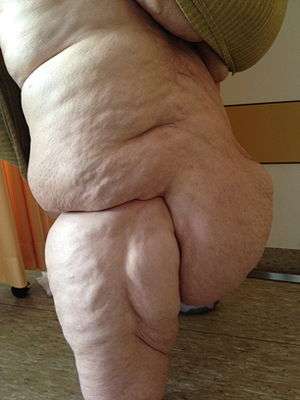 | |
| A very advanced case of lipedema of the right leg (the knee is pointing to the right and is concealed by the overhanging lipedema). | |
| Specialty | Vascular medicine |
| Symptoms | Increased fat deposits under the skin in the legs, easy bruising, pain[1] |
| Causes | Unknown[1] |
| Risk factors | Overweight[1] |
| Differential diagnosis | Obesity, lipohypertrophy, chronic venous insufficiency, lymphedema[1] |
| Treatment | Physiotherapy, exercise[1] |
| Frequency | Up to 11% of women[1] |
The cause is unknown but is believed to involve genetics and hormonal factors.[1] It often runs in families.[1] Risk factors include being overweight or obese.[1] Other conditions that may present similarly include obesity, lipohypertrophy, chronic venous insufficiency, and lymphedema.[1]
A number of treatments may be useful including physiotherapy and exercise. Physiotherapy may help to preserve mobility for a little longer than would otherwise be the case. Exercise, only as much as the patient is able to do without causing damage to the joints, may help with overall fitness but will not prevent progression of the disease.[1] While surgery can remove fat tissue it can also damage lymphatic vessels.[1] Treatment does not typically result in complete resolution.[3] It is estimated to affect up to 11% of women.[1] Onset is typically during puberty, pregnancy, or menopause.[1]
Diagnosis
Differential diagnosis
| Lipedema | Lipo-lymphedema | Lymphedema | Obesity | Venous insufficiency/venous stasis | |
|---|---|---|---|---|---|
| Symptoms: | Fat deposits / swelling in legs and arms not in hands or feet; hands and feet may be affected as the disease progresses. | Fat deposits / swelling widespread in legs/arms/torso | Fat deposits / swelling in one limb including hands and feet | Fat deposits
widespread |
Swelling near ankles; brownish discoloration of lower legs (hemosiderin deposits). Minimal swelling possible. |
| Male/female: | F | F | F/M | F/M | F/M |
| Onset: | Around hormonal shifts (puberty, pregnancy, menopause) | Around hormonal shifts | After surgery that affects lymphatic system, or at birth | Any age | Around onset of obesity, diabetes, pregnancy, hypertension |
| Effects of diet: | Restricting calories ineffective | Restricting calories ineffective | Restricting calories ineffective | Diets and weight loss strategies often effective | No relation to caloric intake |
| Presence of edema: | Non-pitting edema | Lots of edema; some pitting; some fibrosis | Pitting edema | No edema | Often edema, but can also occur without edema in earlier stages |
| Presence of Stemmer Sign: | Stemmer's Sign negative | Stemmer's Sign positive | Stemmer's Sign positive | Stemmer's Sign negative | Stemmer's sign may or may not be present in lymphedema/lipolymphedema |
| Presence of pain: | Pain in affected areas likely | Pain in affected areas | No pain initially | No pain | Pain is likely |
| Affected population: | Best estimate is 11% adult women (study done in Germany) | Unknown; best estimate is a few percent of adult women | Low | >=30% of US adults | >30% of US adults |
| Presence of cellulitis: | No history of cellulitis | Likely history of cellulitis | Possible history of cellulitis | Often itching +/- discoloration mistaken for cellulitis | |
| Family history: | Family history likely | Family history of lipedema likely | Family history not likely unless primary lymphedema | Family history likely | Very likely family history |
Lymphedema
Lipedema can be underdiagnosed due the difficulty in differentiating it from other edemas and obesity, or clinicians failing to make themselves aware of the disease. Trayes 2013 published some tools including tables and a flow chart that can be used to diagnose lipedema and other edemas.[8]
Lipedema / Dercum’s disease differentiation – these conditions may co-exist. Dercum’s disease is characterized by painful lipomas around the body.[9]
Treatment
A number of treatments may be useful including physiotherapy and light exercise which does not put undue stress on the lymphatic system.[1] While surgery can remove fat tissue it can also damage lymphatic vessels.[1] Treatment does not typically result in complete resolution.[3]
The use of surgery to treat the condition is controversial.[3] Options include liposuction and lipectomy.[3]
The studies of highest quality involve tumescent or super tumescent anesthesia and vibrating liposuction, powered, cannula used with lymph sparing techniques.[6][10] The treatment of lipedema with tumescent liposuction requires multiple procedures. In the United States Health Insurance do not generally pay for liposuction for lipedema, making it expensive. Liposuction under general anesthesia, without tumescent anesthesia, can be damaging and is not recommended for the treatment. However, WAL liposuction is an exception. Water Assisted Liposuction developed by Doctor Ziah Taufig from Germany is usually performed under general anesthesia and is considered to be lymphsparing and protective of other tissues such bloodvessels for instance. [11]
Prognosis
Complications include depression, anxiety, and pain.[2]
Epidemiology
Estimates of the incidence of lipedema vary widely, and range as high as 11% of the post-pubertal female population, with estimates of 17 million women in the US, and 370 million women worldwide affected.[7] "11% of adult women" is often cited but that is unsubstantiated.
History
Although first identified in the United States, at the Mayo Clinic in 1940, lipedema is barely known in that country – to physicians or to the patients who have the disease. Lipedema often is confused with obesity, and a significant number of patients currently diagnosed as obese are believed to have lipedema, either instead of or in addition to obesity.[2]
References
- "Lipedema". rarediseases.info.nih.gov. Retrieved 30 December 2016.
- Herbst, Karen L (2012). "Rare adipose disorders (RADs) masquerading as obesity". Acta Pharmacologica Sinica. 33 (2): 155–72. doi:10.1038/aps.2011.153. PMC 4010336. PMID 22301856.
- Warren Peled, A; Kappos, EA (2016). "Lipedema: diagnostic and management challenges". International Journal of Women's Health. 8: 389–95. doi:10.2147/IJWH.S106227. PMC 4986968. PMID 27570465.
- Fat Disorders Research Society Lipedema Description
- Todd, Marie (2010). "Lipoedema: Presentation and management". British Journal of Community Nursing. 15 (4): S10–6. doi:10.12968/bjcn.2010.15.Sup3.47363. PMID 20559170.
- Fife, Caroline E.; Maus, Erik A.; Carter, Marissa J. (2010). "Lipedema". Advances in Skin & Wound Care. 23 (2): 81–92. doi:10.1097/01.ASW.0000363503.92360.91. PMID 20087075.
- Földi, Michael; Földi, Ethel, eds. (2006). "Lipedema". Földi's Textbook of Lymphology. Munich: Elsevier. pp. 417–27. ISBN 978-0-7234-3446-7.
- Trayes, K. P.; Studdiford, J. S.; Pickle, S; Tully, A. S. (2013). "Edema: Diagnosis and management". American Family Physician. 88 (2): 102–10. PMID 23939641.
- http://fatdisorders.org/fat-disorders/diagram%5B%5D
- Langendoen, S.I.; Habbema, L.; Nijsten, T.E.C.; Neumann, H.A.M. (2009). "Lipoedema: From clinical presentation to therapy. A review of the literature". British Journal of Dermatology. 161 (5): 980–6. doi:10.1111/j.1365-2133.2009.09413.x. PMID 19785610.
- Forner-Cordero, I.; Szolnoky, G.; Forner-Cordero, A.; Kemény, L. (2012). "Lipedema: An overview of its clinical manifestations, diagnosis and treatment of the disproportional fatty deposition syndrome - systematic review". Clinical Obesity. 2 (3–4): 86–95. doi:10.1111/j.1758-8111.2012.00045.x. PMID 25586162.
External links
| Classification | |
|---|---|
| External resources |
|