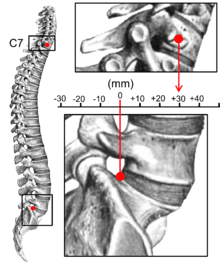
Kyphosis
Kyphosis is an abnormally excessive convex curvature of the spine as it occurs in the thoracic and sacral regions.[1][2] Abnormal inward concave lordotic curving of the cervical and lumbar regions of the spine is called lordosis. It can result from degenerative disc disease; developmental abnormalities, most commonly Scheuermann's disease; osteoporosis with compression fractures of the vertebra; multiple myeloma; or trauma. A normal thoracic spine extends from the 1st to the 12th vertebra and should have a slight kyphotic angle, ranging from 20° to 45°. When the "roundness" of the upper spine increases past 45° it is called kyphosis or "hyperkyphosis". Scheuermann's kyphosis is the most classic form of hyperkyphosis and is the result of wedged vertebrae that develop during adolescence. The cause is not currently known and the condition appears to be multifactorial and is seen more frequently in males than females.[3]
| Hyperkyphosis | |
|---|---|
| Other names | Roundback |
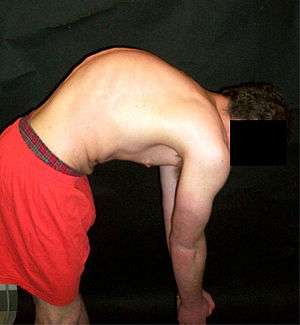 | |
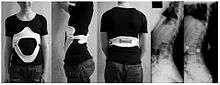
| A preoperative image of a 22-year-old man with Scheuermann's disease, a type of structural kyphosis | |
| Specialty | Orthopedics |
In the sense of a deformity, it is the pathological curving of the spine, where parts of the spinal column lose some or all of their lordotic profile. This causes a bowing of the back, seen as a slouching posture.
While most cases of kyphosis are mild and only require routine monitoring, serious cases can be debilitating. High degrees of kyphosis can cause severe pain and discomfort, breathing and digestion difficulties, cardiovascular irregularities, neurological compromise and, in the more severe cases, significantly shortened life spans. These types of high-end curves typically do not respond well to conservative treatment and almost always warrant spinal fusion surgery, which can restore the body's natural degree of curvature. The term is from Greek κυφός kyphos, a hump.
Signs and symptoms
Complications
The risk of serious complications from spinal fusion surgery for kyphosis is estimated to be 5%, similar to the risks of surgery for scoliosis. Possible complications include inflammation of the soft tissue or deep inflammatory processes, breathing impairments, bleeding, and nerve injuries. According to the latest evidence, the actual rate of complications may be substantially higher. Even among those who do not suffer from serious complications, 5% of patients require reoperation within five years of the procedure, and in general it is not yet clear what one would expect from spine surgery during the long-term.[4][5] Given that the signs and symptoms of spinal deformity cannot be changed by surgical intervention, surgery remains essentially a cosmetic choice.[4][6] However, the cosmetic effects of surgery are not necessarily stable.[4]
Diagnosis
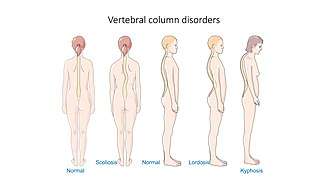
Classification
There are several kinds of kyphosis (ICD-10 codes are provided):
- Postural kyphosis (M40.0), the most common type, normally attributed to slouching, can occur in both the old[7] and the young. In the young, it can be called "slouching" and is reversible by correcting muscular imbalances. In the old, it may be a case of hyperkyphosis and called "dowager's hump". About one third of the most severe hyperkyphosis cases in older people have vertebral fractures.[8] Otherwise, the aging body does tend towards a loss of musculoskeletal integrity,[9] and hyperkyphosis can develop due to aging alone.[8][10]
- Scheuermann's kyphosis (M42.0) is significantly worse cosmetically and can cause varying degrees of pain, and can also affect different areas of the spine (the most common being the midthoracic area). Scheuermann's kyphosis is considered a form of juvenile osteochondrosis of the spine, and is more commonly called Scheuermann's disease. It is found mostly in teenagers and presents a significantly worse deformity than postural kyphosis. A patient suffering from Scheuermann’s kyphosis cannot consciously correct posture.[11][12] The apex of the curve, located in the thoracic vertebrae, is quite rigid. The patient may feel pain at this apex, which can be aggravated by physical activity and by long periods of standing or sitting. This can have a significantly detrimental effect on their lives, as their level of activity is curbed by their condition; they may feel isolated or uneasy amongst peers if they are children, depending on the level of deformity. Whereas in postural kyphosis, the vertebrae and discs appear normal, in Scheuermann’s kyphosis, they are irregular, often herniated, and wedge-shaped over at least three adjacent levels. Fatigue is a very common symptom, most likely because of the intense muscle work that has to be put into standing or sitting properly. The condition appears to run in families. Most patients who undergo surgery to correct their kyphosis have Scheuermann's disease.
- Congenital kyphosis (Q76.4) can result in infants whose spinal column has not developed correctly in the womb. Vertebrae may be malformed or fused together and can cause further progressive kyphosis as the child develops.[13] Surgical treatment may be necessary at a very early stage and can help maintain a normal curve in coordination with consistent follow-ups to monitor changes. However, the decision to carry out the procedure can be very difficult due to the potential risks to the child. A congenital kyphosis can also suddenly appear in teenage years, more commonly in children with cerebral palsy and other neurological disorders.
- Nutritional kyphosis can result from nutritional deficiencies, especially during childhood, such as vitamin D deficiency (producing rickets), which softens bones and results in curving of the spine and limbs under the child's body weight.
- Gibbus deformity is a form of structural kyphosis, often a sequela to tuberculosis.
- Post-traumatic kyphosis (M84.0) can arise from untreated or ineffectively treated vertebral fractures.
Treatments
A diagnosis of kyphosis is generally made through observation and measurement. Idiopathic causes, such as vertebral wedging or other abnormalities, can be confirmed through X-ray. Osteoporosis, a potential cause of kyphosis, can be confirmed with a bone density scan. Postural thoracic kyphosis can often be treated with posture reeducation and focused strengthening exercises. Idiopathic thoracic kyphosis due to vertebral wedging, fractures, or vertebral abnormalities is more difficult to manage, since assuming a correct posture may not be possible with structural changes in the vertebrae. Children who have not completed their growth may show long-lasting improvements with bracing. Exercises may be prescribed to alleviate discomfort associated with overstretched back muscles. A variety of gravity-assisted positions or gentle traction can minimize pain associated with nerve root impingement. Surgery may be recommended for severe idiopathic kyphosis.
Brace
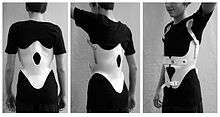
Body braces showed benefit in a randomised controlled trial.[16]
The Milwaukee brace is one particular body brace that is often used to treat kyphosis in the US. Modern CAD/CAM braces are used in Europe to treat different types of kyphosis. These are much easier to wear and have better in-brace corrections than reported for the Milwaukee brace. Since there are different curve patterns (thoracic, thoracolumbar, and lumbar), different types of brace are in use, with different advantages and disadvantages.[15]
Physical therapy
In Germany, a standard treatment for both Scheuermann's disease and lumbar kyphosis is the Schroth method, a system of physical therapy for scoliosis and related spinal deformities.[17] It involves lying supine, placing a pillow under the scapular region and posteriorly stretching the cervical spine.
Surgery
Surgical treatment can be used in severe cases. In patients with progressive kyphotic deformity due to vertebral collapse, a procedure called a kyphoplasty may arrest the deformity and relieve the pain. Kyphoplasty is a minimally invasive procedure,[18] requiring only a small opening in the skin. The main goal is to return the damaged vertebra as close as possible to its original height.[19]
People
- Şehzade Cihangir
- Mahmud I
- Godfrey IV, Duke of Lower Lorraine
- Benjamin Lay
- Georg Christoph Lichtenberg
- Margaret of Bavaria (1442–1479)
- Pepin the Hunchback
- Charles Proteus Steinmetz
See also
- Ehlers–Danlos syndrome
- The Hunchback of Notre-Dame
- The Hunchback of Notre Dame (1996 film)
- Loeys-Dietz syndrome
- Pott's disease
References
- Fon GT, Pitt MJ, Thies AC (May 1980). "Thoracic kyphosis: range in normal subjects". AJR. American Journal of Roentgenology. 134 (5): 979–83. doi:10.2214/ajr.134.5.979. PMID 6768276.
- Voutsinas SA, MacEwen GD (September 1986). "Sagittal profiles of the spine". Clinical Orthopaedics and Related Research (210): 235–42. PMID 3757369.
- "What is Kyphosis?". Your Body Posture. 2018-02-14. Retrieved 2018-02-14.
- Hawes M (2006). "Impact of spine surgery on signs and symptoms of spinal deformity". Pediatric Rehabilitation. 9 (4): 318–39. doi:10.1080/13638490500402264. PMID 17111548.
- Weiss HR, Goodall D (August 2008). "Rate of complications in scoliosis surgery – a systematic review of the Pub Med literature". Scoliosis. 3: 9. doi:10.1186/1748-7161-3-9. PMC 2525632. PMID 18681956.
- Hawes MC, O'Brien JP (2008). "A century of spine surgery: what can patients expect?". Disability and Rehabilitation. 30 (10): 808–17. doi:10.1080/09638280801889972. PMID 18432439.
- Milne JS, Lauder IJ (July 1974). "Age effects in kyphosis and lordosis in adults". Annals of Human Biology. 1 (3): 327–37. doi:10.1080/03014467400000351. PMID 4419577.
- Kado DM, Prenovost K, Crandall C (September 2007). "Narrative review: hyperkyphosis in older persons". Annals of Internal Medicine. 147 (5): 330–8. doi:10.7326/0003-4819-147-5-200709040-00008. PMID 17785488.
- Keller TS, Harrison DE, Colloca CJ, Harrison DD, Janik TJ (March 2003). "Prediction of osteoporotic spinal deformity". Spine. 28 (5): 455–62. doi:10.1097/00007632-200303010-00009. PMID 12616157.
- Chaitow L. "Posture And Correct Body Use". Archived from the original on 8 February 2005.
- "Scoliosis and Spinal Curvatures". Medtronic.
- Nowak JE. Kishner S (ed.). "Scheuermann Disease". Medscape.
- McMaster MJ, Singh H (October 1999). "Natural history of congenital kyphosis and kyphoscoliosis. A study of one hundred and twelve patients". The Journal of Bone and Joint Surgery. American Volume. 81 (10): 1367–83. doi:10.2106/00004623-199910000-00002. PMID 10535587.
- Tebet, Marcos Antonio (2014). "Conceitos atuais sobre equilíbrio sagital e classificação da espondilólise e espondilolistese". Revista Brasileira de Ortopedia. 49 (1): 3–12. doi:10.1016/j.rbo.2013.04.011. ISSN 0102-3616. PMC 4511775. PMID 26229765.
- Weiss, Hans-Rudolf; Turnbull, Deborah (2010). "Kyphosis - Physical and technical rehabilitation of patients with Scheuermann's disease and kyphosis". International Encyclopedia of Rehabilitation.
- Pfeifer M, Begerow B, Minne HW (March 2004). "Effects of a new spinal orthosis on posture, trunk strength, and quality of life in women with postmenopausal osteoporosis: a randomized trial". American Journal of Physical Medicine & Rehabilitation. 83 (3): 177–86. doi:10.1097/01.PHM.0000113403.16617.93. PMID 15043351.
- Lehnert-Schroth, Christa (2007). Three-Dimensional Treatment for Scoliosis: A Physiotherapeutic Method for Deformities of the Spine. Palo Alto, CA: The Martindale Press. pp. 185–187 and passim.
- "Kyphoplasty: Minimally invasive procedure diagrams". Brain And Spine Institute of California. Archived from the original on 2012-05-30.
- "Kyphoplasty". Spine University. Archived from the original on 2011-07-04.
External links
| Classification | |
|---|---|
| External resources |
| Wikimedia Commons has media related to Hunchbacks. |
- Kypho, definition and other related medical terms