Compartment syndrome
Compartment syndrome is a condition in which increased pressure within one of the body's anatomical compartments results in insufficient blood supply to tissue within that space.[6][7] There are two main types: acute and chronic.[6] Compartments of the leg or arm are most commonly involved.[3]
| Compartment syndrome | |
|---|---|
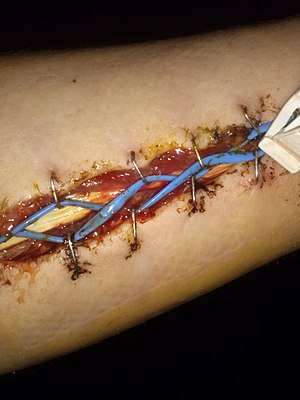 | |
| A picture of the forearm following emergency surgery for acute compartment syndrome. | |
| Specialty | Orthopedics |
| Symptoms | Pain, numbness, pallor, decreased ability to move the affected limb[1] |
| Complications | Acute: Volkmann's contracture[2] |
| Types | Acute, chronic[1] |
| Causes | Acute: Trauma (fracture, crush injury), following a period of poor blood flow[3][4] Chronic: Repetitive exercise[1] |
| Diagnostic method | Based on symptoms, compartment pressure[5][1] |
| Differential diagnosis | Cellulitis, tendonitis, deep vein thrombosis, venous insufficiency[3] |
| Treatment | Acute: Timely surgery[5] Chronic: Physical therapy, surgery[1] |
Symptoms of acute compartment syndrome (ACS) can include severe pain, poor pulses, decreased ability to move, numbness, or a pale color of the affected limb.[5] It is most commonly due to physical trauma such as a bone fracture or crush injury.[3] It can also occur after blood flow returns following a period of poor blood flow.[4] Diagnosis is generally based upon a person's symptoms.[5] Treatment is by surgery to open the compartment completed in a timely manner.[5] If not treated within six hours, permanent muscle or nerve damage can result.[5]
In chronic compartment syndrome, there is generally pain with exercise.[1] Other symptoms may include numbness.[1] Symptoms typically resolve with rest.[1] Common activities that trigger chronic compartment syndrome include running and biking.[1] Generally, this condition does not result in permanent damage.[1] Other conditions that may present similarly include stress fractures and tendinitis.[1] Treatment may include physical therapy or—if that is not effective—surgery.[1]
Acute compartment syndrome occurs in about 3% of those who have a midshaft fracture of the forearm.[8] Rates in other areas of the body and for chronic cases are unknown.[8][9] The condition more often occurs in those under the age of 35 and in males.[3] Compartment syndrome was first described in 1881 by Richard von Volkmann.[5] Untreated, acute compartment syndrome can result in Volkmann's contracture.[2]
Signs and symptoms
Acute compartment syndrome can develop after traumatic injuries, such as in automobile accidents or dynamic sporting activities – for example, a severe crush injury or an open or closed fracture of an extremity. Rarely, ACS can develop after a relatively minor injury, or due to another medical issue.[10] The legs and the forearms are the most frequent sites affected by compartment syndrome. Other areas of the body such as thigh, buttock, hand, and foot can also be affected.[11]
Acute
There are five characteristic signs and symptoms related to acute compartment syndrome: pain, paraesthesia (reduced sensation), paralysis, pallor, and pulselessness.[5] Pain and paresthesia are the early symptoms of compartment syndrome.[11]
- Common
- Pain – A person may experience disproportionate to the findings of the physical examination. This pain may not be relieved by strong analgesic medications. The pain is aggravated by passively stretching the muscle group within the compartment. However, such pain may disappear in the late stages of the compartment syndrome.[11] The role of local anesthesia in delaying the diagnosis of compartment syndrome is still being debated.[11]
- Paresthesia (altered sensation) – A person may complain of "pins & needles", numbness, and a tingling sensation. This may progress to loss of sensation (anesthesia) if no intervention is made.[11]
- Uncommon
- Paralysis – Paralysis of the limb is a rare, late finding. It may indicate both a nerve or muscular lesion.[11]
- Pallor and pulselessness – A lack of pulse rarely occurs in patients, as pressures that cause compartment syndrome are often well below arterial pressures. Absent pulses only occur when there is arterial injury or during the late stages of the compartment syndrome, when compartment pressures are very high.[5] Pallor can also result from arterial occlusion.
The limb affected by compartment syndrome is often associated with a firm, wooden feeling on deep palpation.[5]
Chronic
The symptoms of chronic exertional compartment syndrome, CECS, may involve numbness, tingling, or pain described as burning, cramping, sharp, or stabbing.[12] This pain can occur for months, and in some cases over a period of years, and may be relieved by rest.[12] Moderate weakness in the affected region can also be observed. These symptoms are brought on by exercise and consist of a sensation of extreme tightness in the affected muscles followed by a painful burning sensation if exercise is continued. After exercise is ceased, the pressure in the compartment will decrease within a few minutes, relieving painful symptoms.[12] Symptoms will occur at a certain threshold of exercise which varies from person to person but is rather consistent for a given individual. This threshold can range anywhere from 30 seconds of running to about 10–15 minutes of running. CECS most commonly occurs in the lower leg, with the anterior compartment being the most frequently affected compartment.[12] Foot drop is a common symptom of CECS.[13]
Complications
Failure to relieve the pressure can result in the death of tissues (necrosis) in the affected anatomical compartment, since the ability of blood to enter the smallest vessels in the compartment (capillary perfusion pressure) will fall. This, in turn, leads to progressively increasing oxygen deprivation of the tissues dependent on this blood supply. Without sufficient oxygen, the tissue will die.[14] On a large scale, this can cause Volkmann's contracture in affected limbs, a permanent and irreversible process.[15] Other reported complications include neurological deficits of the affected limb, gangrene, and chronic regional pain syndrome.[16] Rhabdomyolysis and subsequent kidney failure are also possible complications. In some case series, rhabdomyolysis is reported in 23% of patients with ACS.[11]
Causes
Acute
The most common cause of acute compartment syndrome (ACS) is fracture of a bone, which accounts for 69% to 75% of the reported cases. Importantly, there is no difference in the incidence of compartment syndrome between open and closed fractures. Leg compartment syndrome is found in 2% to 9% of tibial fractures. Direct injury to blood vessels can lead to compartment syndrome by reducing the downstream blood supply to soft tissues. This reduction in blood supply can cause a series of inflammatory reactions that promote the swelling of the soft tissues. Such inflammation can be further worsened by reperfusion therapy.[11] Because the fascia layer that defines the compartment of the limbs does not stretch, a small amount of bleeding into the compartment, or swelling of the muscles within the compartment, can cause the pressure to rise greatly. Intravenous drug injection, casts, prolonged limb compression, crush injuries and eschar from burns can also cause compartment syndrome.[17][18] Patients on anticoagulant therapy have an increased risk of bleeding into a closed compartment.[11]
Abdominal compartment syndrome occurs when the intra-abdominal pressure exceeds 20 mmHg and abdominal perfusion pressure is less than 60 mmHg. This disease process is associated with organ dysfunction and multiple organ failures. There are many causes, which can be broadly grouped into three mechanisms: primary (internal bleeding and swelling); secondary (vigorous fluid replacement as an unintended complication of resuscitative medical treatment, leading to the acute formation of ascites and a rise in intra-abdominal pressure); and recurrent (compartment syndrome that has returned after the initial treatment of secondary compartment syndrome).[19]
There have been cases of compartment syndrome associated with hypothyroidism.[20]
Chronic
When compartment syndrome is caused by repetitive use of the muscles, it is known as chronic compartment syndrome (CCS).[21][22] This is usually not an emergency, but the loss of circulation can cause temporary or permanent damage to nearby nerves and muscles.
A subset of chronic compartment syndrome is chronic exertional compartment syndrome (CECS), often called exercise-induced compartment syndrome (EICS).[23] Oftentimes, CECS is a diagnosis of exclusion.[24] CECS of the leg is a condition caused by exercise which results in increased tissue pressure within an anatomical compartment due to an acute increase in muscle volume – as much as 20% is possible during exercise.[25] When this happens, pressure builds up in the tissues and muscles causing tissue ischemia.[25] An increase in muscle weight will reduce the compartment volume of the surrounding fascial borders and result in an increased compartment pressure.[23] An increase in the pressure of the tissue can force fluid to leak into the interstitial space (extracellular fluid), leading to a disruption of the micro-circulation of the leg.[23] This condition occurs commonly in the lower leg and various other locations within the body, such as the foot or forearm. CECS can be seen in athletes who train rigorously in activities that involve constant repetitive actions or motions.[23]
Pathophysiology
In a normal human body, blood flow from the arterial system (higher pressure) to venous system (lower pressure) requires a pressure gradient. When this pressure gradient is diminished, blood flow from the artery to the vein is reduced. This causes a backup of blood and excessive fluid to leak from the capillary wall into spaces between the soft tissues cells, causing swelling of the extracellular space and a rise in intracompartmental pressure. This swelling of the soft tissues surrounding the blood vessels compresses the blood and lymphatic vessels further, causing more fluid to enter the extracellular spaces, leading to additional compression. This worsening cycle can eventually lead to a lack of sufficient oxygen in the soft tissues (tissue ischemia) and tissue death (necrosis). Tingling and abnormal sensation (paraesthesia) can begin as early as 30 minutes from the start of tissue ischemia and permanent damage can occur as early as 12 hours from the onset of the inciting injury.[11]
Diagnosis
Compartment syndrome is a clinical diagnosis, meaning that a medical provider's examination and the patient's history usually give the diagnosis. Apart from the typical signs and symptoms, measurement of intracompartmental pressure can also be important for diagnosis. A transducer connected to a catheter is inserted 5 cm into the zone of injury.[5] A pressure higher than 30 mmHg of the diastolic pressure in a conscious or unconscious person is associated with compartment syndrome. Fasciotomy is indicated in that case. For those patients with low blood pressure (hypotension), a pressure of 20 mmHg higher than the intracompartmental pressure is associated with compartmental syndrome.[11]
Chronic exertional compartment syndrome is usually a diagnosis of exclusion, with the hallmark finding being absence of symptoms at rest. Measurement of intracompartmental pressures during symptom reproduction (usually immediately following running) is the most useful test. Imaging studies (X-ray, CT, MRI) can be useful in ruling out the more common diagnoses.[26]
Treatment
Acute
Any external compression (tourniquet, orthopedic casts or dressings applied on the affected limb) should be removed. Cutting of the cast will reduce the intracompartmental pressure by 65%, followed by 10 to 20% pressure reduction once padding is cut. After removal of the external compression the limb should be placed at the level of the heart. The vital signs of the patient should be closely monitored. If the clinical condition does not improve, then fasciotomy is indicated to decompress the compartments. An incision large enough to decompress all the compartments is necessary. This surgical procedure is performed inside an operating theater under general or local anesthesia.[11] The timing of the fasciotomy wound closure is debated. Some surgeons suggest wound closure would done seven days after fasciotomy.[11]
Chronic
Treatment for chronic exertional compartment syndrome can include decreasing or subsiding exercise and/or exacerbating activities, massage, non-steroidal anti-inflammatory medication, and physiotherapy. Chronic compartment syndrome in the lower leg can be treated conservatively or surgically. Conservative treatment includes rest, anti-inflammatory medications, and manual decompression. Elevation of the affected limb in patients with compartment syndrome is contraindicated, as this leads to decreased vascular perfusion of the affected region. Ideally, the affected limb should be positioned at the level of the heart. The use of devices that apply external pressure to the area, such as splints, casts, and tight wound dressings, should be avoided.[27] If symptoms persist after conservative treatment or if an individual does not wish to give up the physical activities which bring on symptoms, compartment syndrome can be treated by a surgery known as a fasciotomy.
A US military study conducted in 2012 found that teaching individuals with lower leg chronic exertional compartment syndrome to change their running style to a forefoot running technique abated symptoms in those with symptoms limited to the anterior compartment.[28] Running with a forefoot strike limits use of the tibialis anterior muscle which may explain the relief in symptoms in those with anterior compartment syndrome.
Hyperbaric oxygen therapy has been suggested by case reports – though as of 2011 not proven in randomized control trials – to be an effective adjunctive therapy for crush injury, compartment syndrome, and other acute traumatic ischemias, by improving wound healing and reducing the need for repetitive surgery.[29][30]
Prognosis
A mortality rate of 47% has been reported for acute compartment syndrome of the thigh. According to one study the rate of fasciotomy for acute compartment syndrome varied from 2% to 24%.[11] The most significant prognostic factor in patients with acute compartment syndrome is time to diagnosis.[10]
Epidemiology
In one case series of 164 patients diagnosed with acute compartment syndrome, 69% of the cases had an associated fracture. The authors of that article also calculated an annual incidence of acute compartment syndrome of 1 to 7.3 per 100,000.[31] There are significant differences in the incidence of acute compartment syndrome based on age and gender. With a similar injury pattern, an older patient is more likely to develop ACS than a younger person.[10] Men are ten times more likely than women to develop ACS. The mean age for ACS in men is 30 years while the mean age is 44 years for women.[11]
See also
References
- "Compartment Syndrome-OrthoInfo – AAOS". www.orthoinfo.org. October 2009. Archived from the original on 14 March 2017. Retrieved 29 July 2017.
- El-Darouti MA (2013). Challenging Cases in Dermatology. Springer Science & Business Media. p. 145. ISBN 9781447142492. Archived from the original on 2017-07-29.
- Ferri FF (2017). Ferri's Clinical Advisor 2018 E-Book: 5 Books in 1. Elsevier Health Sciences. p. 317. ISBN 9780323529570. Archived from the original on 2017-07-29.
- Schmidt AH (July 2016). "Acute Compartment Syndrome". The Orthopedic Clinics of North America. 47 (3): 517–25. doi:10.1016/j.ocl.2016.02.001. PMID 27241376.
- Donaldson J, Haddad B, Khan WS (2014). "The pathophysiology, diagnosis and current management of acute compartment syndrome". The Open Orthopaedics Journal. 8: 185–93. doi:10.2174/1874325001408010185. PMC 4110398. PMID 25067973.
- "Compartment Syndrome – National Library of Medicine". PubMed Health. Archived from the original on 10 September 2017. Retrieved 25 July 2017.
- Peitzman AB, Rhodes M, Schwab CW (2008). The Trauma Manual: Trauma and Acute Care Surgery. Lippincott Williams & Wilkins. p. 349. ISBN 9780781762755. Archived from the original on 2017-07-29.
- Bucholz RW (2012). Rockwood and Green's Fractures in Adults: Two Volumes Plus Integrated Content Website (Rockwood, Green, and Wilkins' Fractures). Lippincott Williams & Wilkins. p. 691. ISBN 9781451161441. Archived from the original on 2017-07-29.
- Miller MD, Wiesel SW (2012). Operative Techniques in Sports Medicine Surgery. Lippincott Williams & Wilkins. p. 437. ISBN 9781451124903. Archived from the original on 2017-07-29.
- Taylor RM, Sullivan MP, Mehta S (September 2012). "Acute compartment syndrome: obtaining diagnosis, providing treatment, and minimizing medicolegal risk". Current Reviews in Musculoskeletal Medicine. 5 (3): 206–13. doi:10.1007/s12178-012-9126-y. PMC 3535085. PMID 22644598.
- Via AG, Oliva F, Spoliti M, Maffulli N (2015). "Acute compartment syndrome". Muscles, Ligaments and Tendons Journal. 5 (1): 18–22. PMC 4396671. PMID 25878982.
- Bong MR, Polatsch DB, Jazrawi LM, Rokito AS (2005). "Chronic exertional compartment syndrome: diagnosis and management" (PDF). Bulletin. 62 (3–4): 77–84. PMID 16022217.
- Awbrey B, Shingo T. "Chronic Exercise-Induced Compartment Syndrome of the Leg". Harvard Orthopaedic Journal. 1 (7). Archived from the original on 24 September 2015. Retrieved 16 October 2014.
- Shears E, Porter K (October 2006). "Acute compartment syndrome of the limb". Trauma. 8 (4): 261–266. doi:10.1177/1460408606076963.
- Eichler GR, Lipscomb PR (January 1967). "The changing treatment of Volkmann's ischemic contractures from 1955 to 1965 at the Mayo Clinic". Clinical Orthopaedics and Related Research. 50: 215–23. doi:10.1097/00003086-196701000-00022. PMID 6029018.
- Kalyani, B. S.; Fisher, B. E.; Roberts, C. S.; Giannoudis, P. V. (2011). "Journal of Hand Surgery". www.jhandsurg.org. 36 (3): 535–43. doi:10.1016/j.jhsa.2010.12.007. PMID 21371630. Retrieved 2018-12-14.
- Konstantakos EK, Dalstrom DJ, Nelles ME, Laughlin RT, Prayson MJ (December 2007). "Diagnosis and management of extremity compartment syndromes: an orthopaedic perspective". The American Surgeon. 73 (12): 1199–209. PMID 18186372.
- Salcido R, Lepre SJ (October 2007). "Compartment syndrome: wound care considerations". Advances in Skin & Wound Care. 20 (10): 559–65, quiz 566–7. doi:10.1097/01.ASW.0000294758.82178.45. PMID 17906430.
- Maerz L, Kaplan LJ (April 2008). "Abdominal compartment syndrome". Critical Care Medicine. 36 (4 Suppl): S212–5. doi:10.1097/CCM.0b013e318168e333. PMID 18382196.
- Adams, James G. (2012). Emergency Medicine E-Book: Clinical Essentials (Expert Consult -- Online). Elsevier Health Sciences. p. 797. ISBN 9781455733941.
- Wanich T, Hodgkins C, Columbier JA, Muraski E, Kennedy JG (December 2007). "Cycling injuries of the lower extremity". The Journal of the American Academy of Orthopaedic Surgeons. 15 (12): 748–56. doi:10.5435/00124635-200712000-00008. PMID 18063715.
- Verleisdonk EJ (October 2002). "The exertional compartment syndrome: A review of the literature". Ortopedia, Traumatologia, Rehabilitacja. 4 (5): 626–31. PMID 17992173.
- Cetinus E, Uzel M, Bilgiç E, Karaoguz A, Herdem M (April 2004). "Exercise induced compartment syndrome in a professional footballer". British Journal of Sports Medicine. 38 (2): 227–9. doi:10.1136/bjsm.2003.004630. PMC 1724759. PMID 15039267.
- Liu B, Barrazueta G, Ruchelsman DE (November 2017). "Chronic Exertional Compartment Syndrome in Athletes". The Journal of Hand Surgery. 42 (11): 917–923. doi:10.1016/j.jhsa.2017.09.009. PMID 29101975.
- Touliopolous S, Hershman EB (March 1999). "Lower leg pain. Diagnosis and treatment of compartment syndromes and other pain syndromes of the leg". Sports Medicine. 27 (3): 193–204. doi:10.2165/00007256-199927030-00005. PMID 10222542.
- Blackman PG (March 2000). "A review of chronic exertional compartment syndrome in the lower leg". Medicine and Science in Sports and Exercise. 32 (3 Suppl): S4–10. doi:10.1249/00005768-200003001-00002. PMID 10730989.
- Meyer RS, White KK, Smith JM, Groppo ER, Mubarak SJ, Hargens AR (October 2002). "Intramuscular and blood pressures in legs positioned in the hemilithotomy position : clarification of risk factors for well-leg acute compartment syndrome". The Journal of Bone and Joint Surgery. American Volume. 84-A (10): 1829–35. PMID 12377915.
- Diebal AR, Gregory R, Alitz C, Gerber JP (May 2012). "Forefoot running improves pain and disability associated with chronic exertional compartment syndrome". The American Journal of Sports Medicine. 40 (5): 1060–7. doi:10.1177/0363546512439182. PMID 22427621.
- Undersea and Hyperbaric Medical Society. "Crush Injury, Compartment syndrome, and other Acute Traumatic Ischemias". Archived from the original on 2008-05-08.
- Bouachour G, Cronier P, Gouello JP, Toulemonde JL, Talha A, Alquier P (August 1996). "Hyperbaric oxygen therapy in the management of crush injuries: a randomized double-blind placebo-controlled clinical trial". The Journal of Trauma. 41 (2): 333–9. doi:10.1097/00005373-199608000-00023. PMID 8760546.
- McQueen MM, Gaston P, Court-Brown CM (March 2000). "Acute compartment syndrome. Who is at risk?". The Journal of Bone and Joint Surgery. British Volume. 82 (2): 200–3. doi:10.1302/0301-620X.82B2. PMID 10755426.
External links
| Classification | |
|---|---|
| External resources |
| Wikimedia Commons has media related to Compartment syndrome. |
- Compartment Syndrome of the Forearm – Orthopaedia.com
- Chronic Exertional Compartment Syndrome detailed at MayoClinic.com
- Compartment_syndrome at the Duke University Health System's Orthopedics program
- 05-062a. at Merck Manual of Diagnosis and Therapy Home Edition
- Compartment syndrome
- American Association of Orthopaedic Surgeons Compartment Syndrome